Introduction
Have you ever wondered whether you are actually ovulating, or why so many people say to “track your temperature” when trying to understand fertility? For many women, basal body temperature (often called BBT) sounds simple at first: take your temperature every morning and look for a pattern. But once you begin, the questions quickly follow. What counts as a temperature rise? Does BBT predict ovulation or only confirm it? And what happens if stress, poor sleep, illness, or shift work gets in the way?
Basal body temperature tracking can be a useful way to learn more about your menstrual cycle, especially when combined with other signs, such as cervical mucus and cycle length. But it also has limitations, and it is important to understand both what it can show and what it cannot. Reputable guidance from the NHS, ACOG, and NICE makes clear that body temperature changes may help identify fertile patterns, but BBT alone is not a reliable way to predict ovulation in real time, and it is not recommended as a stand-alone medical test to confirm normal ovulation. (nhs.uk)
What is basal body temperature?
Basal body temperature is your body’s lowest resting temperature, usually measured first thing in the morning after sleep and before getting out of bed, talking, eating, or drinking. The idea behind BBT tracking is that hormone changes across the menstrual cycle influence your resting temperature in a small but measurable way. After ovulation, progesterone rises, and this hormone has a warming effect on the body. That is why many women notice a slight upward shift in temperature after the egg has already been released. (NCBI)
This means BBT is best understood as a retrospective sign of ovulation. In other words, it usually tells you that ovulation has likely happened, rather than warning you clearly before it happens. ACOG notes that body temperature typically rises slightly around the time of ovulation. At the same time, NICE advises that basal body temperature charts do not reliably predict ovulation and should not be used as a stand-alone method to confirm whether someone is ovulating normally in a clinical setting. (ACOG)
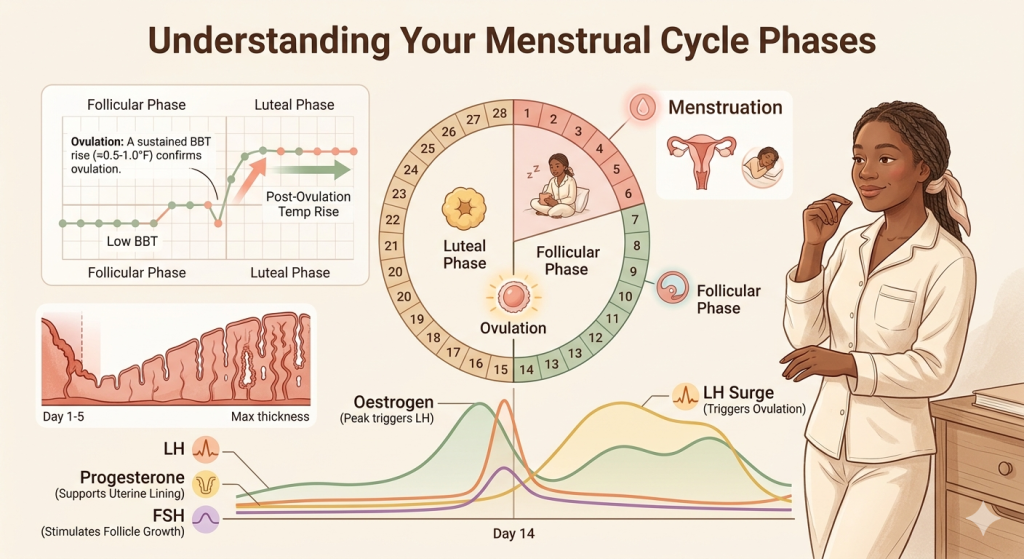
How BBT changes during the menstrual cycle
The menstrual cycle is driven by a finely coordinated conversation between the brain, ovaries, and reproductive hormones. In the first half of the cycle, called the follicular phase, oestrogen is more dominant and resting temperatures tend to be lower. Around ovulation, luteinizing hormone triggers the release of an egg. After ovulation, the ruptured follicle becomes the corpus luteum, which produces progesterone. Progesterone raises resting body temperature, creating the classic biphasic chart pattern many fertility trackers look for. (NCBI)
Research summaries in NCBI and related peer-reviewed reviews describe this rise as small, often around 0.3°C to 0.7°C across the post-ovulatory phase. Some consumer guidance describes it as roughly 0.5°F to 1°F. The key point is that the change is usually subtle, not dramatic, which is why a sensitive basal thermometer and consistent timing matter. (PMC)
How to track basal body temperature properly
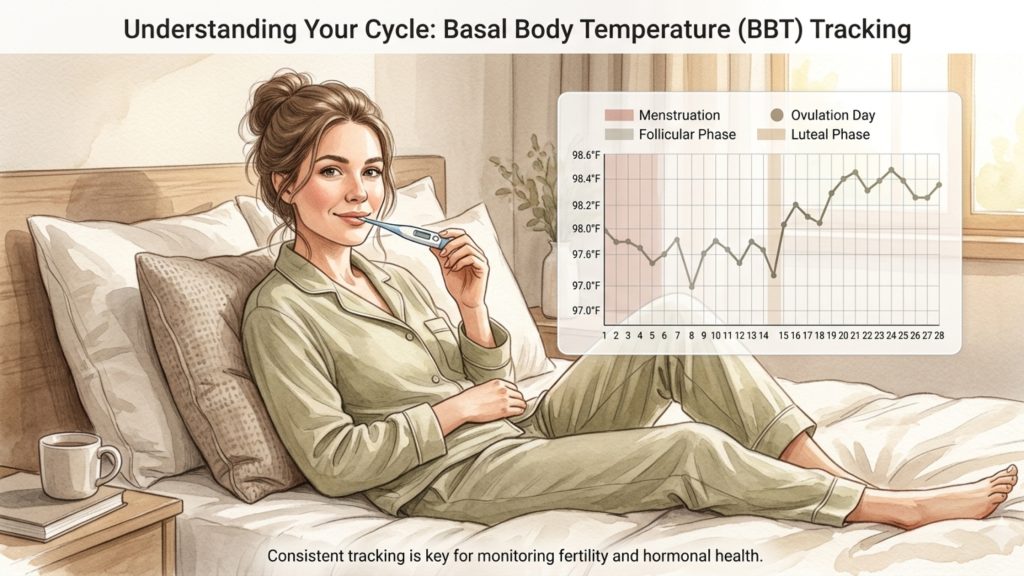
To get meaningful information from BBT, consistency matters more than perfection. Take your temperature immediately after waking, before sitting up or moving around. Use the same thermometer each day, preferably a basal thermometer that measures to two decimal places. Record the reading daily and track it over several cycles rather than expecting a clear answer in just a few days. The NHS notes that fertility awareness methods usually take a few cycles to learn properly. (nhs.uk)
Many people chart BBT using an app, paper chart, or fertility journal. What you are usually watching for is a sustained rise that remains elevated for at least several days after the lower temperatures of the earlier cycle phase. This pattern may suggest that ovulation has already occurred. Some women also notice other ovulation-related body signs around the same time, including wetter, clearer, more slippery cervical mucus before ovulation. Combining these signs is generally more useful than relying on temperature alone. (nhs.uk)
Earliest Signs of Pregnancy: What They Mean and When to Test
What BBT can and cannot tell you
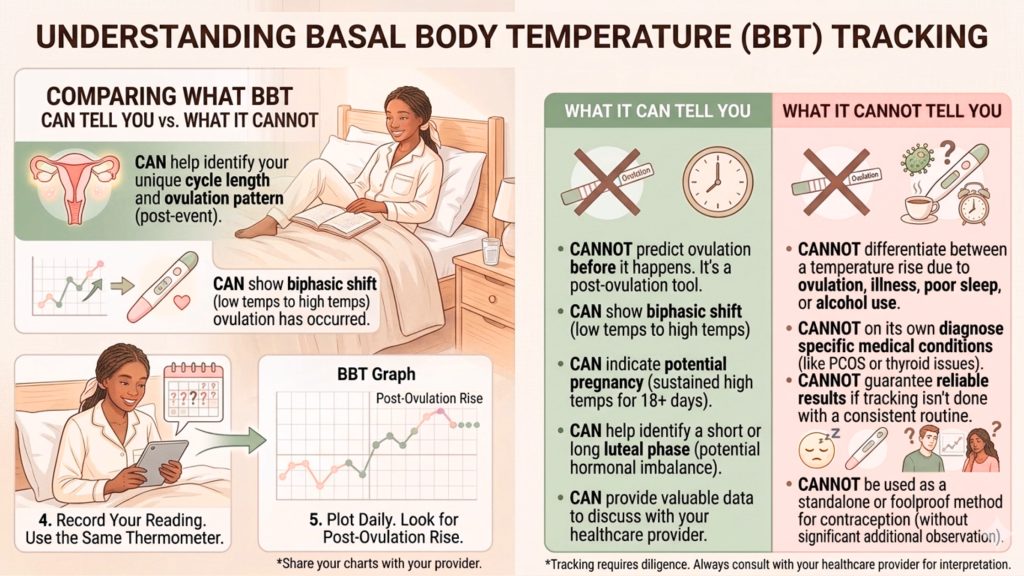
BBT tracking can help you become more aware of your cycle pattern. Over time, it may help you spot whether you tend to have a post-ovulatory temperature shift, whether your cycles appear broadly consistent, and when your luteal phase begins. This can be reassuring for some women who are trying to conceive or want to understand their hormonal rhythm better. (NCBI)
But it is just as important to understand its limits. BBT does not pinpoint the exact hour of ovulation. It does not reliably predict ovulation before it happens. It can also be thrown off by interrupted sleep, illness, fever, alcohol, travel, jet lag, night shifts, certain medications, stress, and inconsistent measurement habits. NHS fertility awareness guidance specifically notes that fertility signals can be affected by illness, stress, and travel, and local NHS sexual health guidance advises not to rely on a single fertility indicator alone. (nhs.uk)
That makes BBT a helpful pattern-tracking tool, but not a perfect fertility test. If someone has irregular cycles, suspected anovulation, or difficulty conceiving, clinical assessment is more reliable than temperature charts alone. NICE recommends hormone testing, including progesterone testing timed to the cycle, rather than depending on BBT charts to confirm ovulation. (NICE)
Factors that can affect your readings
Several real-life factors can make a BBT chart harder to interpret. Poor sleep is a common problem, especially for new parents, shift workers, and anyone under prolonged stress. Acute illness and fever can raise readings. Alcohol the night before may do the same. Travel across time zones, sleeping later than usual, waking up repeatedly, or taking the temperature after getting out of bed can all blur the pattern. (nhs.uk)
Underlying health conditions may matter too. Irregular cycles, thyroid disorders, polycystic ovary syndrome, perimenopause, and some medications can affect ovulation patterns or make charting less straightforward. BBT can still be recorded in these situations, but the results may be less predictable and should not replace professional evaluation when symptoms or fertility concerns are present. NICE and NHS fertility guidance support further assessment when cycles are irregular or conception is not happening as expected. (NICE)
Practical guidance for using BBT well
If you want to use BBT meaningfully, think of it as one piece of a bigger picture. Pair it with cycle tracking and cervical mucus observations. Look for trends over at least two to three cycles. Keep notes beside your temperatures for anything that may have affected a reading, such as poor sleep, fever, alcohol, or stress. (nhs.uk)
For women trying to conceive, BBT may help reveal when ovulation probably happened in previous cycles, which can help with timing intercourse earlier in the fertile window next time. For contraception, fertility awareness methods need proper teaching and should not be improvised casually, because timing errors can easily happen. The NHS advises learning fertility awareness with a trained professional. (nhs.uk)
Common myths and misconceptions
Myth 1: A temperature rise predicts ovulation before it happens
Usually, it does not. In most cases, the rise occurs after ovulation because progesterone levels are higher after the egg is released. (NCBI)
Myth 2: One high reading means you ovulated
Not necessarily. Illness, broken sleep, alcohol, or measuring at a different time can all distort a single reading. A pattern matters more than one number. (nhs.uk)
Myth 3: BBT alone is enough for everyone
No. Both NHS and sexual health guidance support using more than one fertility sign, and NICE does not recommend BBT as a reliable stand-alone clinical method to confirm ovulation. (gwh.nhs.uk)
When to seek medical advice
Speak to a doctor or fertility specialist if your periods are very irregular, you rarely have periods, your charts never show a clear temperature shift, or you have been trying to conceive without success. NICE guidance supports fertility assessment when pregnancy has not happened after regular unprotected sex over time, and earlier review may be appropriate if there are known reproductive health concerns. Seek help sooner if you have symptoms such as severe pelvic pain, very heavy bleeding, symptoms of thyroid disease, or a history of PCOS, endometriosis, or pelvic infection. (NICE)
FAQs
Does BBT confirm ovulation?
It may suggest that ovulation has likely occurred when you see a sustained rise, but NICE says it is not a reliably recommended clinical method to confirm ovulation on its own. (NICE)
When should I take my basal body temperature?
Take it immediately after waking, before getting out of bed, eating, drinking, or talking much. (NCBI)
How much does the temperature rise after ovulation?
Often only slightly, commonly around 0.3°C to 0.7°C or roughly 0.5°F to 1°F. (PMC)
Can I use BBT to get pregnant?
It can help you understand past ovulation patterns, but it works best alongside cervical mucus tracking and other methods. (nhs.uk)
Can stress affect BBT?
Yes. Stress, illness, disrupted sleep, and travel can all affect readings. (nhs.uk)
Is BBT useful if my periods are irregular?
It may still be informative, but charts are often harder to interpret. Irregular cycles deserve a proper medical assessment if ovulation is uncertain. (NICE)
Is a normal BBT chart proof of fertility?
No. A chart pattern alone cannot assess egg quality, tubal patency, sperm factors, or wider reproductive health. (NICE)
Medical disclaimer
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment. Basal body temperature tracking can offer useful cycle insights, but it is not a substitute for professional assessment. If you have irregular periods, difficulty conceiving, severe symptoms, or concerns about ovulation, speak with a qualified healthcare professional.