Introduction: Healing After a C-Section Can Feel Like a Lot
If you have recently had a caesarean birth, you may be asking yourself: Is this pain normal? Should my incision look like that? Why am I still so tired? When should I call someone?
C-section recovery symptoms can feel confusing because you are healing from two big things at once: childbirth and major abdominal surgery. On top of that, you may also be feeding a baby, sleeping in short bursts, managing bleeding, coping with hormonal shifts, and trying to understand what your body is telling you.
Some soreness, tiredness, bleeding, swelling, and pulling around the incision are common in the first few weeks and can help reassure you about normal healing. But symptoms such as fever, worsening pain, heavy bleeding, chest pain, shortness of breath, a swollen, painful leg, or an incision that is leaking fluid should never be ignored. Major organisations such as ACOG, the CDC, Mayo Clinic, NHS, and March of Dimes all advise seeking medical help for specific postpartum warning signs. (ACOG)
This guide will walk you through common C-section recovery symptoms, what they usually mean, what to expect, and when to call a doctor.
What Is It?
A C-section, or caesarean section, is a surgical birth where a baby is delivered through an incision made in the abdomen and uterus. Because it is surgery, recovery usually takes longer than recovery after an uncomplicated vaginal birth. The NHS notes that many women need to take things easy for several weeks after a caesarean, while the March of Dimes states that full recovery often takes around 4 to 6 weeks.
When we talk about C-section recovery symptoms, we mean the physical and emotional changes that can happen as your body heals after surgery and birth. These may include:
- Incision pain or tenderness
- Abdominal soreness
- Vaginal bleeding
- Swelling in the feet or legs
- Constipation or trapped wind
- Fatigue
- Breast tenderness or milk coming in
- Mood changes
- Difficulty moving comfortably
- Numbness or tingling near the scar
Some symptoms are part of normal healing. Others can be signs of infection, blood clots, heavy bleeding, blood pressure problems, or postpartum mood disorders.
Swollen Legs After Childbirth: What’s Normal and When to Worry
Why Does It Happen?
Your body is healing from surgery.
During a C-section, several layers of tissue are opened or moved to reach the uterus. Even when the operation goes smoothly, your muscles, skin, nerves, blood vessels, and uterus all need time to heal. That is why coughing, laughing, standing up, or turning in bed can feel surprisingly sore in the early days.
Your uterus is shrinking back down.
After birth, the uterus contracts to return to its pre-pregnancy size. These cramps, sometimes called afterpains, can feel stronger during breastfeeding because oxytocin helps the uterus contract. This can be uncomfortable but is often a normal part of postpartum recovery.
Your hormones are shifting quickly.
Oestrogen and progesterone drop after birth. These changes can affect sweating, mood, sleep, skin, appetite, and emotions. It is common to feel tearful or overwhelmed in the early days, but persistent sadness, anxiety, panic, hopelessness, or thoughts of harming yourself or your baby need urgent support. ACOG and March of Dimes both list thoughts of self-harm or harm to the baby as serious postpartum warning signs. (ACOG)
Your blood clot risk is higher.
Pregnancy and childbirth naturally increase the risk of clotting, and surgery can further increase it. Mayo Clinic explains that C-section birth may increase the risk of deep vein thrombosis, especially in the legs or pelvis; if a clot travels to the lungs, it can become life-threatening. (Mayo Clinic)
This does not mean you should panic. Symptoms such as a painful, swollen leg, chest pain, or shortness of breath require immediate medical attention, as they could indicate serious complications like blood clots or pulmonary issues.
Evidence-Based Solutions
1. Take pain relief as advised
Pain control matters. When pain is managed effectively, you can breathe deeply, walk gently, feed your baby more comfortably, and rest better. Following your clinician’s advice on pain relief options, such as paracetamol or ibuprofen, can make a significant difference in your recovery experience.
Common options may include:
- Paracetamol/acetaminophen
- Ibuprofen or other anti-inflammatory medication, if suitable for you
- Short-term stronger pain relief if prescribed
- Using a pillow to support your abdomen when coughing, laughing, or standing
Do not wait until pain becomes severe before taking prescribed medication unless your doctor has told you otherwise.
2. Check your incision daily
Mayo Clinic recommends checking your C-section incision for signs of infection. Call your healthcare professional if the wound becomes red or swollen, leaks fluid, changes colour, or develops a fever.
Look for:
- Increasing redness or warmth
- Swelling around the wound
- Pus, fluid, or bad-smelling discharge
- Worsening pain instead of gradual improvement
- Opening of the wound
- Fever or chills
For darker skin tones, redness may look more like purple, brown, or grey, or show a larger colour change.
3. Move gently but regularly
Gentle walking helps circulation, reduces stiffness, and may lower the risk of constipation and blood clots. Mayo Clinic Health System notes that walking after C-section can support recovery and help prevent constipation and potentially dangerous clots. (Mayo Clinic Health System)
Start small. A short walk to the bathroom or a quick walk around the room counts.
Keeping your follow-up appointments is a key part of feeling supported during recovery. These visits are an opportunity to discuss bleeding, pain, mood, blood pressure symptoms, feeding, contraception, pelvic floor health, and emotional well-being, helping you feel cared for and monitored. Your postpartum check is not just a “quick scar check.” It is an opportunity to discuss bleeding, pain, mood, blood pressure symptoms, feeding, contraception, pelvic floor health, and emotional well-being.
Medical Interventions: When Treatment May Be Needed
Most C-section recovery symptoms improve with time, rest, wound care, and pain relief. But some symptoms need medical treatment.
A doctor may recommend:
- Antibiotics for wound infection or uterine infection
- Blood pressure treatment if postpartum hypertension or preeclampsia is suspected
- Blood tests or scans if there are signs of infection, bleeding, or clots
- Blood-thinning medication if a clot is diagnosed
- Wound care or drainage if the incision opens or forms an abscess
- Mental health support or medication for postpartum depression, anxiety, or trauma symptoms
The NHS lists wound infection, womb lining infection, heavy bleeding, and blood clots as possible C-section risks, with symptoms such as wound redness, swelling, increasing pain, discharge, fever, tummy pain, abnormal discharge, and heavy bleeding. (nhs.uk)
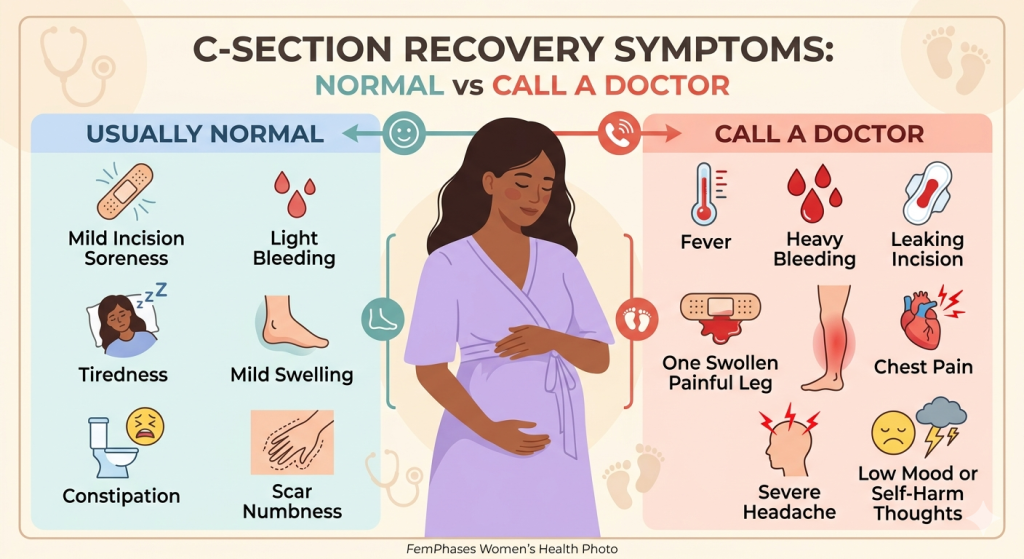
Signs or Symptoms
Common C-section recovery symptoms
These can be normal, especially if they gradually improve:
- Mild to moderate discomfort from the incision
- Tenderness or pulling around the scar
- Tiredness and low energy
- Light to moderate vaginal bleeding
- Small clots in the first few days
- Mild swelling in both feet or ankles
- Constipation or trapped gas
- Numbness around the scar
- Cramping as the uterus shrinks
- Difficulty standing fully upright at first
Symptoms that need attention
These are not symptoms to “push through”:
- Fever of 38°C / 100.4°F or higher
- Worsening abdominal pain
- Incision redness, swelling, leaking, or opening
- Heavy bleeding that soaks a pad in an hour
- Large blood clots
- Bad-smelling vaginal discharge
- One swollen, painful, warm, or red leg
- Chest pain or shortness of breath
- Severe headache or vision changes
- Dizziness, fainting, or feeling very unwell
- Thoughts of harming yourself or your baby
The CDC lists urgent maternal warning signs, including fever, severe headache, dizziness or fainting, vision changes, extreme swelling, chest pain, trouble breathing, and thoughts of self-harm. (CDC)
What Is Normal and When to Pay Attention
i. Incision pain
Normal: Soreness, tightness, pulling, or burning sensations that slowly improve.
Pay attention: Pain that gets worse, becomes severe, or comes with redness, swelling, discharge, fever, or wound opening.
ii. Vaginal bleeding
Normal: Bleeding that gradually becomes lighter, changing from red to pink or brown, then yellowish-white.
Pay attention: Bleeding that soaks through more than one pad per hour, large clots, bleeding that suddenly becomes heavy again, or feeling faint. Mayo Clinic lists soaking more than one pad an hour or passing egg-sized clots as warning signs. (Mayo Clinic)
iii. Swelling
Normal: Mild swelling in both legs or feet, especially in the first week, often from pregnancy fluid shifts and IV fluids.
Pay attention: One leg that is swollen, painful, warm, or changed in colour. This may be a sign of a clot. (Mayo Clinic)
iv. Tiredness
Normal: Feeling exhausted, especially with sleep disruption and surgery recovery.
Pay attention: Extreme weakness, fainting, shortness of breath, racing heart, or feeling unable to function.
v. Mood changes
Normal: Tearfulness, emotional sensitivity, and mood swings in the first couple of weeks.
Pay attention: Persistent sadness, panic, frightening thoughts, hopelessness, feeling detached from the baby, or thoughts of self-harm.

Holistic and Lifestyle Changes
These steps will not replace medical care, but they can support healing.
a. Nutrition for tissue repair
Your body needs fuel to rebuild tissue and restore energy. Focus on:
- Protein: eggs, fish, chicken, beans, lentils, tofu, yoghurt
- Iron-rich foods: red meat, spinach, beans, fortified cereals
- Vitamin C foods: oranges, berries, peppers, tomatoes
- Fibre: oats, vegetables, fruit, whole grains
- Fluids: water, soups, herbal teas, especially if breastfeeding
b. Support your scar gently.
Follow your hospital’s wound care instructions. Keep the area clean and dry, avoid tight waistbands, and do not use creams, oils, or scar massage until the wound is fully closed and your provider says it is safe.
c. Protect your abdomen
For the first few weeks:
- Avoid heavy lifting beyond your baby unless advised otherwise
- Roll onto your side before getting out of bed
- Hold a pillow over your incision when coughing or laughing
- Avoid intense abdominal exercises until cleared
d. Rest without guilt
Rest is not laziness. It is treatment. C-section recovery symptoms often worsen when women try to do too much too soon.
When to See a Doctor
Call your doctor, midwife, maternity triage, or urgent care service if you notice:
- Fever of 38°C / 100.4°F or higher
- Incision redness, swelling, warmth, leaking, bad smell, or opening
- Pain that is worsening rather than improving
- Heavy bleeding, soaking a pad in an hour
- Large clots or sudden return of bright red bleeding
- Bad-smelling vaginal discharge
- Burning when passing urine or difficulty urinating
- One leg that is painful, swollen, warm, red, purple, or changed in colour
- Severe headache, vision changes, or swelling of the face/hands
- Chest pain, shortness of breath, coughing blood, or gasping for air
- Fainting, seizures, confusion, or feeling seriously unwell
- Thoughts of harming yourself, your baby, or feeling unsafe
Seek emergency help immediately for chest pain, trouble breathing, seizures, severe bleeding, or thoughts of self-harm. ACOG and the CDC both highlight these as serious postpartum warning signs. (ACOG)
Key Takeaway
Most C-section recovery symptoms—such as soreness, tiredness, mild swelling, light bleeding, and scar tenderness—are expected in the first few weeks and should gradually improve. The keyword is improve. If symptoms are getting worse, feel severe, or come with fever, heavy bleeding, wound changes, chest pain, shortness of breath, one-sided leg swelling, severe headache, or worrying mood symptoms, call a healthcare professional promptly.
You are not overreacting by asking for help. After a C-section, your body deserves careful attention, not silent endurance.

Frequently Asked Questions
1. What C-section recovery symptoms are normal in the first week?
Common C-section recovery symptoms in the first week include incision soreness, abdominal tenderness, vaginal bleeding, tiredness, trapped wind, constipation, mild swelling, and difficulty moving comfortably. These should slowly improve, not get worse.
2. How long does C-section recovery usually take?
Many women feel noticeably better after a few weeks, but full recovery often takes around 4 to 6 weeks. Some people need longer, especially if they have complications, infection, anaemia, poor sleep, or limited support at home.
3. When should I worry about my C-section incision?
Call a doctor if the incision becomes more painful, red, swollen, hot, leaks fluid or pus, smells bad, opens, bleeds heavily, or if you develop a fever. These can be signs of infection or delayed wound healing. (Mayo Clinic)
4. Is it normal to feel numb around my C-section scar?
Yes, numbness, tingling, or altered sensation around the scar can happen because small nerves are affected during surgery. It often improves slowly, but some numbness may last longer. Mention it at your check-up, especially if it’s accompanied by worsening pain or swelling.
5. Is heavy bleeding normal after a C-section?
Some bleeding is normal because the uterus still sheds its lining after birth. Heavy bleeding is not normal. Seek medical advice if you soak more than one pad an hour, pass large clots, feel faint, or if bleeding suddenly becomes much heavier. (Mayo Clinic)
6. Can C-section recovery symptoms include anxiety or low mood?
Yes. Hormonal changes, pain, sleep loss, birth trauma, and the demands of newborn care can affect mood. But intense anxiety, panic, ongoing sadness, hopelessness, or thoughts of harming yourself or your baby need urgent support.
7. What helps C-section recovery symptoms improve safely?
Gentle walking, good pain control, hydration, fibre, protein-rich meals, wound care, rest, and accepting help can all support healing. But lifestyle care should not replace medical help if warning signs appear.
Medical Disclaimer
This article is for general education only and is not a substitute for personal medical advice, diagnosis, or treatment. C-section recovery can vary from person to person. If you have severe symptoms, feel something is not right, or are worried about your incision, bleeding, pain, breathing, leg swelling, headache, mood, or safety, contact your doctor, midwife, maternity unit, urgent care service, or emergency services immediately.



