Introduction:
Constipation during menopause can feel like one more uncomfortable thing your body has suddenly decided to do without asking your permission. You may feel bloated, heavy, sluggish, or frustrated because your bowel routine no longer feels predictable. And when it happens alongside hot flashes, sleep changes, mood shifts, weight changes, or fatigue, it can leave us wondering: “Is this menopause, my diet, stress, or something else?”
The reassuring answer is this: constipation during menopause is common, but it is not something you have to put up with. Hormonal changes can affect digestion, but so can fibre intake, hydration, movement, stress, medication, pelvic floor changes, thyroid problems, and underlying bowel conditions.
In this article, we’ll gently walk through why constipation during menopause happens, what symptoms to look for, what may be considered common, when to get checked, and the practical steps that can help you feel more comfortable and regular again.
What Is Constipation?
Constipation means your bowel movements are less frequent, harder to pass, or feel incomplete. You don’t need to go every day. For some people, three times a week may be normal. What matters is whether your usual pattern has changed, whether stools are hard or painful, and whether you feel blocked, bloated, or unable to fully empty your bowels.
The NHS describes constipation as having fewer bowel movements than usual, straining, passing hard or lumpy stools, or feeling that you have not fully emptied your bowel. It can happen at any age, but it becomes more common with changes in routine, diet, activity, medication, and life stage.
During perimenopause and menopause, digestion can become more sensitive. Some women notice constipation, bloating, gas, reflux, abdominal discomfort, or alternating constipation and diarrhoea. Women’s Health Concern, part of the British Menopause Society, notes that hormonal changes during menopause, including declining oestrogen, may influence the gut microbiome and gut-brain communication.
So, constipation during menopause is not “all in your head.” Your gut, hormones, nervous system, sleep, stress levels, and lifestyle are all connected.
What Are the First Signs of Menopause? Early Symptoms to Notice
Why Does It Happen?
i. Hormonal Changes Can Slow Digestion
Oestrogen and progesterone do not only affect periods, fertility, or hot flashes. They also interact with the digestive system. During perimenopause, hormones can fluctuate unpredictably. Later, as oestrogen levels decline, some women notice changes in bowel movement, bloating, and gut sensitivity.
This does not mean hormones are always the only cause. But hormone changes may make the bowel more reactive, slower, or more sensitive than before.
ii. Stress and the Gut-Brain Axis
The gut and brain are in constant conversation. This is often called the gut-brain axis. When we are stressed, anxious, grieving, overwhelmed, or sleeping badly, digestion can slow down or become irregular.
Many women reach midlife carrying a lot: work, caring roles, ageing parents, teenagers, relationship changes, body changes, and emotional pressure. The bowel often responds to that load.
iii. Lower Activity Levels
Movement helps stimulate bowel motility. If menopause symptoms are making you tired, achy, low in mood, or less active, constipation can become more likely. Sitting for long periods can also slow digestion.
iv. Changes in Food, Fibre, and Fluid Intake
Constipation during menopause can be linked to insufficient fibre intake, inadequate fluid intake, or reduced consumption of whole foods. Some women reduce their food intake when trying to manage weight changes, which may unintentionally reduce fibre intake and stool bulk.
Fibre helps stool hold water and move through the bowel more easily. But increasing fibre too quickly can worsen bloating, so it is best to build up slowly.
v. Medication and Supplements
Some medicines and supplements can cause or worsen constipation, including:
- Opioid painkillers, such as codeine
- Some antidepressants
- Some blood pressure medicines
- Iron tablets
- Some antihistamines
- Some bladder medications
- Some antacids
- Calcium supplements in some people
The NHS advises speaking to a doctor before stopping any prescribed medication that may be contributing to constipation.
vi. Pelvic Floor Changes
Pregnancy, childbirth, ageing, menopause, chronic coughing, heavy lifting, and reduced oestrogen can affect pelvic floor strength and coordination. Sometimes the issue is not only stool consistency, but difficulty relaxing or coordinating the pelvic floor when trying to empty the bowel.
This can create a sensation of blockage, incomplete emptying, or needing to strain.
vii. Other Medical Causes
Constipation during menopause may also be caused or worsened by medical conditions, such as:
- Underactive thyroid
- Diabetes
- Irritable bowel syndrome
- Coeliac disease
- Bowel inflammation
- Neurological conditions
- Pelvic organ prolapse
- Bowel obstruction, rarely
- Bowel cancer, rarely
This is why new, persistent, or worsening constipation should not be dismissed as “just menopause.”
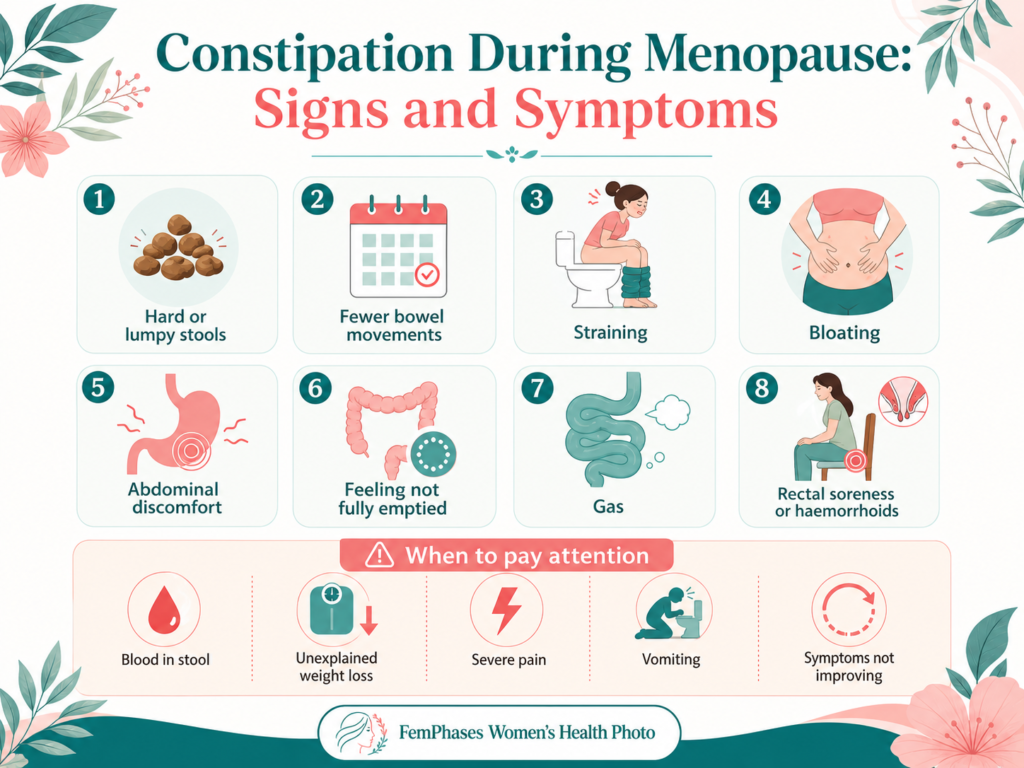
Signs and Symptoms
Constipation during menopause may show up in obvious and less obvious ways.
Common symptoms include:
- Going to the toilet less often than usual
- Hard, dry, or lumpy stools
- Straining to pass stool
- Feeling as if stool is stuck
- Feeling like you have not fully emptied your bowel
- Bloating or abdominal pressure
- Cramping or discomfort
- Passing more wind than usual
- Nausea or reduced appetite
- Feeling heavy, sluggish, or uncomfortable
- Haemorrhoids or soreness from straining
- Small tears around the anus, known as fissures
- Needing to sit on the toilet for a long time
Some women also notice that constipation becomes worse:
- Before a period during perimenopause
- During stressful weeks
- After poor sleep
- While travelling
- After increasing protein but not fibre
- After starting iron, pain medication, or other new medication
What Is Normal and When to Pay Attention?
Constipation can happen occasionally and may improve with simple changes. But it deserves attention if it is new, persistent, painful, or comes with other symptoms.
1. Common Changes
These changes may be common during menopause, but they are still worth monitoring:
- Occasional constipation during stressful periods
- Mild bloating with slower bowel movements
- Hard stools after drinking less fluid
- Constipation after travel or routine changes
- Symptoms after reducing fibre or movement
- Constipation linked to a new medication or supplement
- Mild changes around hormonal fluctuations in perimenopause
ii. Needs Urgent Attention
Please speak to a healthcare professional if you notice:
- Blood in your stool
- Unexplained weight loss
- Constipation that does not improve with treatment
- Regular or worsening constipation
- Persistent bloating
- Ongoing tummy pain
- Feeling tired all the time, especially with constipation
- A sudden change in bowel habit
- Constipation after starting a medication
- Vomiting, severe swelling, or inability to pass wind
- Symptoms of anaemia, such as dizziness, weakness, breathlessness, or unusual fatigue
The NHS recommends seeing a healthcare professional if constipation is not improving with treatment, occurs regularly, is accompanied by bloating, blood in the stool, unexplained weight loss, tiredness, tummy pain, or a sudden change in bowel habit.

Evidence-Based Solutions
Relief depends on the cause, severity, age, medical history, menopause stage, medication use, pregnancy possibility, and personal preferences. The best approach is usually gentle, steady, and realistic rather than extreme.
a. Start With Your Pattern
Before changing everything at once, track:
- How often you open your bowels
- Stool type, using the Bristol Stool Chart if helpful
- Straining or pain
- Bloating or cramps
- Fluid intake
- Fibre intake
- New medication or supplements
- Stress and sleep
- Menopause symptoms
- Any bleeding, weight loss, or red flags
This gives you and your healthcare professional a clearer picture.
Heavy periods in your 40s: causes, signs, and what helps
b. Medical Interventions
i. Doctor or Nurse Assessment
If constipation during menopause is new, regular, severe, or not improving, your doctor or nurse may ask about your bowel pattern, diet, fluid intake, medication, menstrual or menopause history, weight changes, bleeding, pain, and family history.
They may examine your abdomen and, where appropriate, discuss rectal examination, blood tests, stool tests, or referral.
ii. Blood Tests
Depending on your symptoms, blood tests may check for:
- Anaemia
- Thyroid function
- Inflammation
- Diabetes markers
- Coeliac disease
- Kidney function or calcium levels, where relevant
iii. Medication Review
If constipation began after starting a medication or supplement, your clinician may review the dose, timing, or alternatives. Do not stop prescribed medication without advice.
iv. Laxatives
Laxatives can be helpful when lifestyle changes are not enough. Different types work in different ways:
- Bulk-forming laxatives increase stool bulk and require adequate fluid intake.
- Osmotic laxatives help draw water into the bowel.
- Stimulant laxatives encourage bowel movement.
- Stool softeners may help if stools are hard and painful.
NICE guidance for adults recommends gradually increasing laxative doses to achieve comfortable bowel movements with soft, formed stools.
HRT and Menopause Care
Hormone replacement therapy, or HRT, is not usually prescribed specifically for constipation. However, if you have broader menopause symptoms such as hot flashes, night sweats, sleep disturbance, vaginal symptoms, mood changes, or joint aches, it may be worth discussing menopause treatment options with a qualified clinician.
The British Menopause Society states that for many healthy women under 60, or within a few years of menopause, the benefits of HRT for clear menopause indications often outweigh the risks, depending on the person’s individual health profile.
Holistic and Lifestyle Support
i. Increase Fibre Slowly
Fibre is one of the most useful supports for constipation during menopause, but sudden big changes can make bloating worse. Increase gradually over days to weeks.
Helpful fibre sources include:
- Oats
- Lentils and beans
- Vegetables
- Berries
- Apples and pears
- Chia seeds or ground flaxseed
- Wholegrain bread or brown rice
- Nuts and seeds
- Prunes or kiwi fruit for some people
Aim for consistency rather than perfection.
ii. Drink Enough Fluid
Fibre needs fluid to work well. If you increase fibre but do not drink enough, stools may become harder.
A simple starting point is to notice the colour of your urine. Pale yellow usually suggests better hydration, while dark urine may suggest you need more fluid, unless it’s due to vitamins or medication.
iii. Move Your Body Daily
You do not need intense workouts to support bowel health. Try:
- A 10–20 minute walk
- Gentle stretching
- Yoga or Pilates
- Light strength training
- Taking movement breaks if you sit for long periods
Movement supports bowel motility, mood, sleep, blood sugar balance, and long-term health.
iv. Support Your Toilet Routine
Small changes can make a big difference:
- Try going after breakfast, when the bowel is naturally more active.
- Do not ignore the urge to go.
- Place your feet on a small stool so your knees are slightly higher than your hips.
- Lean forward with elbows on knees.
- Breathe slowly rather than holding your breath.
- Avoid prolonged straining.
v. Manage Stress Gently
Because the bowel responds to the nervous system, calming practices can help some women. Try:
- Slow breathing
- A short walk outside
- Journaling
- Gentle stretching before bed
- Reducing multitasking where possible
- Therapy or support if stress, anxiety, grief, or trauma feels heavy
This does not mean constipation is “caused by stress alone.” It means your gut may need support from your nervous system, too.
vi. Be Careful With Supplements
Some supplements can help, but they can also cause side effects or interact with medicines. Magnesium may help some people with constipation, but it is not suitable for everyone, especially those with kidney disease or certain medication risks. Iron can worsen constipation, so speak with a clinician if you need iron but struggle with your bowels.
Avoid treating supplements as cures. Use them thoughtfully and check with a pharmacist, doctor, or qualified clinician if you are unsure.
When to See a Doctor
Please seek medical advice if constipation during menopause is persistent, worsening, painful, or unusual for you.
Seek urgent medical help if you have:
- Severe abdominal pain
- Vomiting with constipation
- A swollen or hard abdomen
- Inability to pass stool or wind
- Fainting
- Chest pain
- Shortness of breath
- Sudden weakness
- Heavy bleeding
- Bleeding after sex
- Bleeding after menopause
- New breast changes
- Unexplained weight loss
- Symptoms of anaemia
- Pregnancy concerns
- Severe mood changes
- Thoughts of self-harm
Even if you suspect menopause is involved, it is always safer to check symptoms that feel new, severe, or not right for your body.
Key Takeaway
Constipation during menopause is common, but it should not be ignored or brushed aside. Hormonal shifts can affect digestion, but constipation may also be linked to fibre intake, fluid intake, movement, stress, medication, pelvic floor changes, thyroid problems, or bowel conditions.
Track your bowel pattern, stool changes, bloating, pain, medication, and any red flags. Start with gentle, practical steps: more fibre, enough fluid, daily movement, a better toilet position, and stress support. If symptoms persist or worsen, or if they come with warning signs, speak with a healthcare professional.
Not sure where your symptoms fit? Take the Tools and Quizzes to understand your pattern.

Frequently Asked Questions
1. Is constipation during menopause normal?
Constipation during menopause is common, but “common” does not mean it should be ignored. If it is new, persistent, painful, or comes with bleeding, weight loss, tiredness, or a sudden bowel change, speak with a healthcare professional.
2. Can low oestrogen cause constipation?
Low or fluctuating oestrogen may contribute to digestive changes by influencing gut function, the gut microbiome, and gut-brain communication. However, constipation can have multiple causes, including diet, fluid intake, activity, medication, and stress.
3. What helps constipation during menopause naturally?
Helpful steps include gradually increasing fibre intake, drinking enough fluids, moving daily, responding to the urge to go, improving toilet posture, reducing straining, and managing stress. If symptoms do not improve, medical advice is important.
4. What foods are good for menopause constipation?
Oats, beans, lentils, vegetables, fruit, berries, prunes, kiwi, chia seeds, ground flaxseed, wholegrains, nuts, and seeds may help. Increase fibre slowly to reduce bloating.
5. Can HRT help constipation during menopause?
HRT is not usually used as a direct treatment for constipation. But if constipation occurs alongside other menopause symptoms, such as hot flashes, poor sleep, mood changes, or vaginal symptoms, it may be worth discussing menopause care and treatment options with your clinician.
6. When should I worry about constipation?
Seek medical advice if constipation is regular, worsening, not improving, or associated with blood in stool, unexplained weight loss, persistent bloating, tummy pain, tiredness, anaemia symptoms, or sudden bowel habit changes.
7. Are laxatives safe during menopause?
Laxatives can be safe and helpful when used appropriately, but the best type depends on your symptoms and medical history. Ask a pharmacist, doctor, or nurse if you are unsure, especially if you take other medications or have ongoing symptoms.
Medical Disclaimer
This article is for educational purposes only and does not replace personalised medical advice, diagnosis, or treatment. If you are worried about your symptoms, if your symptoms are getting worse, or if something does not feel right in your body, please speak with your doctor, nurse practitioner, gynaecologist, endocrinologist, or another qualified healthcare professional. Seek urgent medical help for severe, sudden, or concerning symptoms.