Introduction
If you’re trying to conceive after 35, one question can start to sit heavily in the background: Have I left it too late? For many women, this season comes with a mix of hope, pressure, and conflicting advice. You may hear that everything suddenly becomes difficult at 35, or that age matters little at all. The truth sits somewhere in the middle. Fertility does change with age, but 35 is not a cliff edge, and many women do conceive in their mid-to-late 30s and beyond. (CDC)
Quick answer:
Trying to conceive after 35 often means pregnancy may take longer, and it is worth being a bit more proactive sooner. What does not change is that regular ovulation, well-timed sex, good preconception health, and checking in early if something feels off still matter most. If you are 35 or older and have been trying for 6 months without pregnancy, it is sensible to speak to a doctor. (ASRM)
What is it?
Trying to conceive after 35 means attempting pregnancy in a stage of life when fertility is gradually becoming less efficient than it was in the 20s and early 30s. It does not mean infertility by default. It means the odds of conception per cycle are lower than before, and the time-to-pregnancy may be longer. (ASRM)
What changes after 35?
- The number of eggs in the ovaries continues to decline
- Egg quality also changes with age
- Ovulation may still happen regularly, but conception can take longer
- The risk of miscarriage and chromosomal problems rises with age (acog.org)
What does not change?
- You still only need one healthy egg, one healthy sperm, and the right timing
- A healthy cycle still matters
- Your partner’s fertility still matters too
- Good pre-pregnancy care can still make a meaningful difference (CDC)
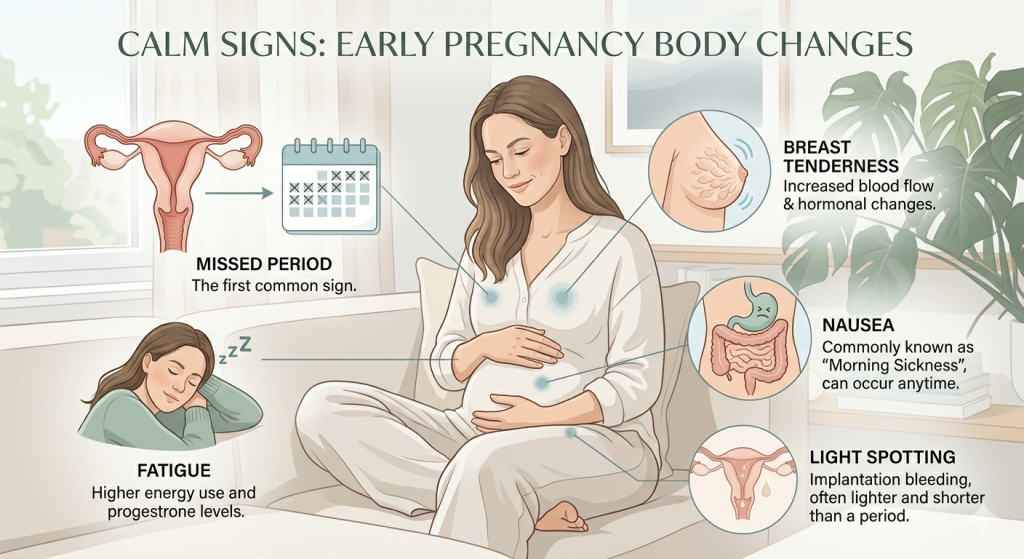
Earliest Signs of Pregnancy: What They Mean and When to Test
Why does it happen?
The main reason trying to conceive after 35 can look different is age-related ovarian change. Women are born with all the eggs they will ever have. Over time, both the number and quality of those eggs decline. That decline becomes more noticeable in the mid-30s, though it remains gradual and highly individual. (CDC)

The biggest biological reasons
Egg quantity
There are fewer eggs available over time, so the chance of releasing an egg that leads to pregnancy becomes lower. (CDC)
Egg quality
As eggs age, chromosome errors become more common. This can make conception harder and increase the risk of miscarriage. ACOG notes that clinically recognised early pregnancy loss rises from about 20% at age 35 to about 40% at age 40. (acog.org)
Other health factors
At 35 and beyond, it is also more common to have issues that can affect fertility, such as endometriosis, fibroids, thyroid problems, blocked tubes, or conditions that affect ovulation. Male fertility can also decline with age, especially after age 40. (CDC)
Signs or symptoms
Trying to conceive after 35 does not always come with obvious symptoms. Many women have regular periods and feel completely well. Still, some signs may indicate it’s worth checking in earlier.
Signs everything may still be on track
- Regular menstrual cycles
- Clear signs of ovulation, such as predictable cycle patterns
- No history of pelvic infection, major pelvic surgery, or endometriosis
- No known sperm concerns in a partner (CDC)
Signs worth paying attention to
- Very irregular periods or no periods
- Very painful periods
- Known endometriosis or PCOS
- Previous pelvic inflammatory disease or STI complications
- Recurrent miscarriage
- A history of chemotherapy, pelvic surgery, or fertility problems
- A male partner with known sperm issues or testicular problems (ASRM)
What is normal, and when to pay attention
This is often the part women most want clarified. Trying to conceive after 35 does not mean panic at month one or two. It is still normal for pregnancy to take a little time.
What is usually normal
It can take several months.
Even in healthy couples, pregnancy does not usually happen instantly. Timing, ovulation, and chance all play a role. Intercourse every 1 to 2 days during the fertile window gives the highest pregnancy rates, though 2 to 3 times a week is often nearly as effective and easier to sustain. (ASRM)
A bit more planning helps.
When trying to conceive after 35, it helps to:
- Take 400 micrograms of folic acid daily
- Stop smoking
- Avoid alcohol while trying to conceive
- Review medicines with a doctor
- Aim for a healthy weight
- Track cycles if that helps you identify your fertile window (nhs.uk)
Cramping in Early Pregnancy: What Is Normal and What Is Not?
When to pay attention sooner
If you are 35 or older, most expert guidance suggests seeking assessment after 6 months of regular, unprotected sex without pregnancy, rather than waiting a full year. If you are over 40 or you already know you may have a fertility issue, it is reasonable to seek help even sooner. (ASRM)
When to speak to a doctor
You do not need to wait until things feel desperate.
Make an appointment sooner if:
- You are trying to conceive after 35, and 6 months have passed without pregnancy
- You are over 40
- Your periods are irregular, absent, or very painful
- You have had 2 or more miscarriages
- You or your partner has a known fertility-related condition
- You have thyroid disease, diabetes, or another long-term condition
- You take regular medication and want to know if it is pregnancy-safe (acog.org)
What a doctor may do
Early fertility review
A doctor or fertility specialist may review your cycle pattern, medical history, medications, lifestyle, and your partner’s health, too. Fertility is never only a “woman’s issue.” (CDC)
Tests may include
- Blood tests to look at ovulation and hormones
- A semen analysis for a partner
- Imaging or further checks to see if there are signs of blocked tubes, fibroids, or endometriosis (ASRM)

Key takeaway
Trying to conceive after 35 does bring real changes, but not hopeless ones. The biggest difference is usually timing: pregnancy may take longer, and it makes sense to act a little sooner if it is not happening. What does not change is the value of good cycle timing, preconception care, and early support when needed. If you are trying to conceive after 35, the goal is not to panic. It is to be informed, realistic, and gently proactive. (ASRM)
Frequently Asked Questions
Q: Can you still get pregnant naturally at 35, 37, or 39?
A: Yes. Many women do. Trying to conceive after 35 may take longer, but a natural pregnancy is still possible for many women in their late 30s. (CDC)
Q: Is age 35 really a fertility cliff?
A: Not exactly. Fertility declines gradually, not overnight. Age 35 matters because the decline becomes more noticeable, not because fertility suddenly stops. (CDC)
Q: How long should I try before getting help after 35?
A: Most guidance recommends speaking to a doctor after 6 months of trying if you are 35 or older. (ASRM)
Q: Does regular monthly ovulation mean my fertility is fine?
A: Not always. Regular periods are reassuring, but they do not rule out egg quality issues, tubal problems, endometriosis, or sperm factors. (CDC)
Q: What can I do to improve my chances of conceiving after 35?
A: Have sex every 1 to 2 days during the fertile window, take folic acid, stop smoking, avoid alcohol, review medicines, and seek help sooner if pregnancy is not happening. (ASRM)
Q: Does my partner’s age matter too?
A: Yes. Male fertility also changes with age, and male factors contribute to infertility as well. (CDC)
Q: Is miscarriage more common after 35?
A: Yes. The risk rises with age, largely because chromosomal problems become more common in eggs over time. (acog.org)
Medical Disclaimer
This article is for general education only and is not a diagnosis or a substitute for personal medical care. If you are trying to conceive after 35 and have concerns about your cycle, fertility, miscarriage, or underlying health conditions, speak to your doctor, OB-GYN, or a fertility specialist for advice tailored to you. If you have severe pain, very irregular periods, repeated pregnancy loss, or are over 40 and trying to conceive, seek medical guidance promptly.