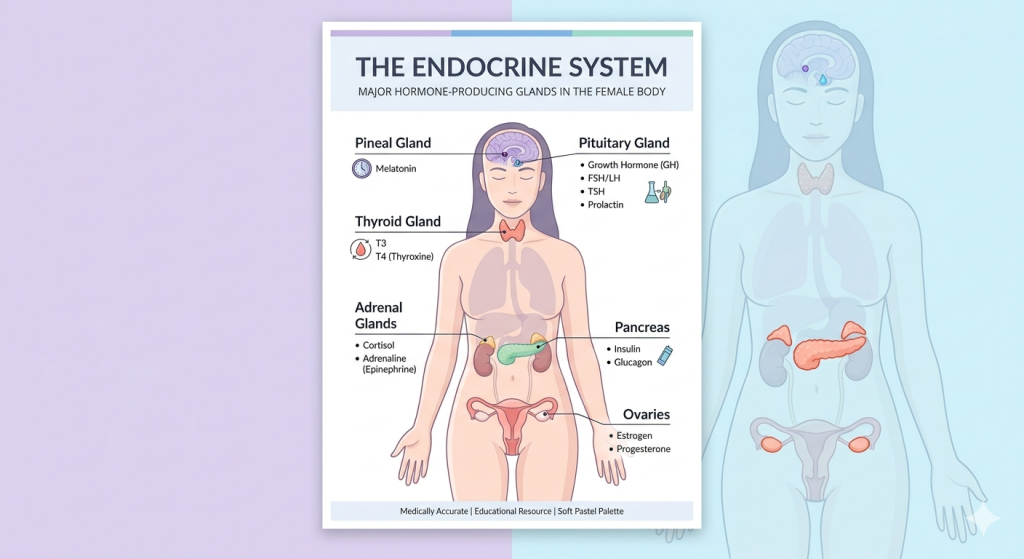
Introduction
Have you ever felt like your skin follows your cycle more closely than your calendar does? Your breakouts flare before a period, worsen during times of stress, or appear out of nowhere in adulthood. That pattern can feel frustrating, especially when you are doing “all the right things” and still waking up to painful, under-the-skin spots.
Hormonal acne is not a formal medical diagnosis, but it is a useful everyday term for acne that appears to be strongly influenced by hormonal shifts. Acne itself is a very common skin condition. The NHS says it affects most people at some point, often causing spots, oily skin, and, in some cases, tender or painful skin. Adult acne can be especially common in women, and hormone changes around periods, pregnancy, and conditions such as polycystic ovary syndrome, or PCOS, are recognised triggers. (nhs.uk)
What is hormonal acne?
Hormonal acne is acne driven or worsened by hormonal changes, especially androgens. Androgens are hormones present in both sexes, but when their effects are stronger, they can stimulate the sebaceous glands to produce more sebum. More sebum, combined with sticky skin cells and inflammation inside the hair follicle, creates the conditions for acne lesions to form. (PMC)
In practical terms, hormonal acne often shows up as recurring breakouts along the lower face, jawline, and chin, and sometimes the neck, though acne can affect the face, chest, and back as well. It may include blackheads and whiteheads, but many women describe deeper, more inflamed spots that feel sore and take longer to settle. Severe acne can also lead to scarring or post-inflammatory marks. (British Association of Dermatologists)
How hormones influence the skin
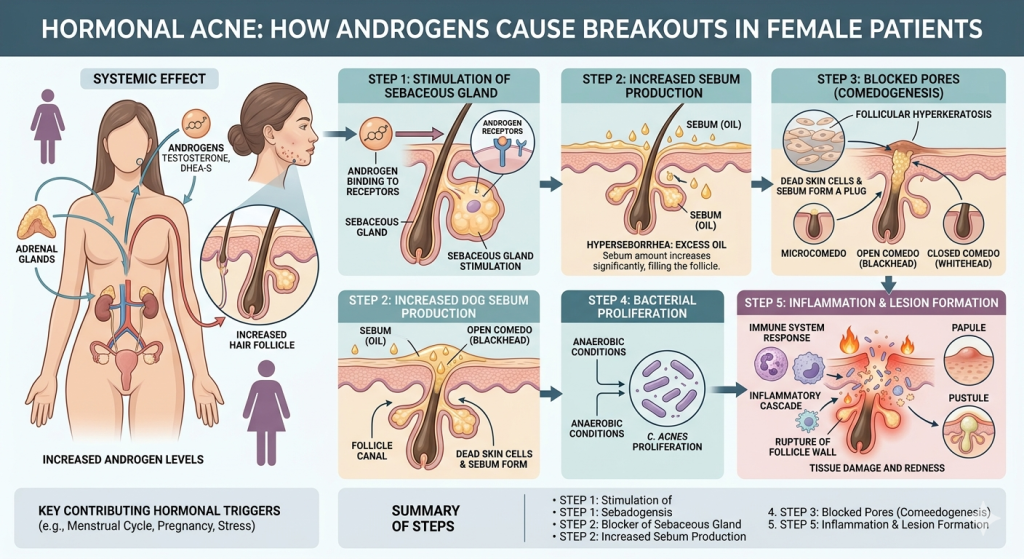
Androgens, sebum, and blocked pores
Biology begins in the pilosebaceous unit, which includes the hair follicle and oil gland. Acne is now understood as a chronic inflammatory disorder of the skin. Androgens such as testosterone and dihydrotestosterone, or DHT, stimulate sebaceous gland activity. In some women, acne is linked not only to high androgen levels but also to skin glands being unusually sensitive to normal hormone levels. That means blood tests can sometimes look normal even when the skin is clearly reacting in a hormone-sensitive way. (NCBI)
Once excess oil is produced, dead skin cells can accumulate and clog the follicle. This creates microcomedones, the earliest acne lesions. Inside that plugged, oil-rich space, inflammation develops, and Cutibacterium acnes can contribute to the process. Importantly, this bacterium is part of the normal skin microbiome, so acne is not simply “dirty skin.” The problem is the combination of oil, blockage, inflammation, and shifts in the skin environment. (PMC)
Why breakouts can follow hormonal life stages
Hormonal acne often becomes more obvious during puberty because androgen activity rises. In women, it may also flare around menstruation, pregnancy, perimenopause, or with PCOS. The NHS specifically notes that many cases of adult female acne are thought to be linked to hormone changes, especially around periods and pregnancy, and hormonal conditions such as PCOS can also be involved. (nhs.uk)
Signs and symptoms to look out for
Hormonal acne does not always look the same. However, common features include breakouts that flare in a pattern, acne that worsens before a period, tender, inflamed spots on the chin or jawline, oily skin, and acne that persists or begins in adulthood. Some people also notice blackheads, whiteheads, papules, pustules, or deeper nodules. The NHS and dermatology sources note that acne severity can range from a few comedones to painful nodules and cyst-like lesions, with the potential for scarring in more severe cases. (nhs.uk)
If acne is accompanied by irregular periods, increased facial hair, scalp hair thinning, weight changes, or fertility concerns, that raises the question of an underlying hormonal issue, such as PCOS and deserves medical review. Hyperandrogenism is a recognised driver of acne in some adult women. (nhs.uk)
Influencing factors: age, stress, lifestyle, and health conditions
Hormones are central, but they are not the whole story. Age matters because acne commonly starts in adolescence, yet it can continue into adult life, and the NHS notes that a smaller proportion of adults over 35 still experience acne. Adult female acne is well recognised in clinical literature. (nhs.uk)
Stress does not directly “cause” acne, but it may worsen inflammation and flare-prone skin. Diet is more nuanced than many internet claims suggest. NICE includes advice on diet in acne care, and research reviews suggest that higher-glycaemic-load diets may be associated with acne in some people. However, diet is not the sole cause, and responses vary from person to person. (NICE)
Certain medicines, skincare habits, friction from helmets or masks, and picking at spots can also worsen acne or increase the risk of marks and scarring. PCOS is an important related condition in women with persistent acne, especially when menstrual symptoms or signs of androgen excess are also present. (NICE)
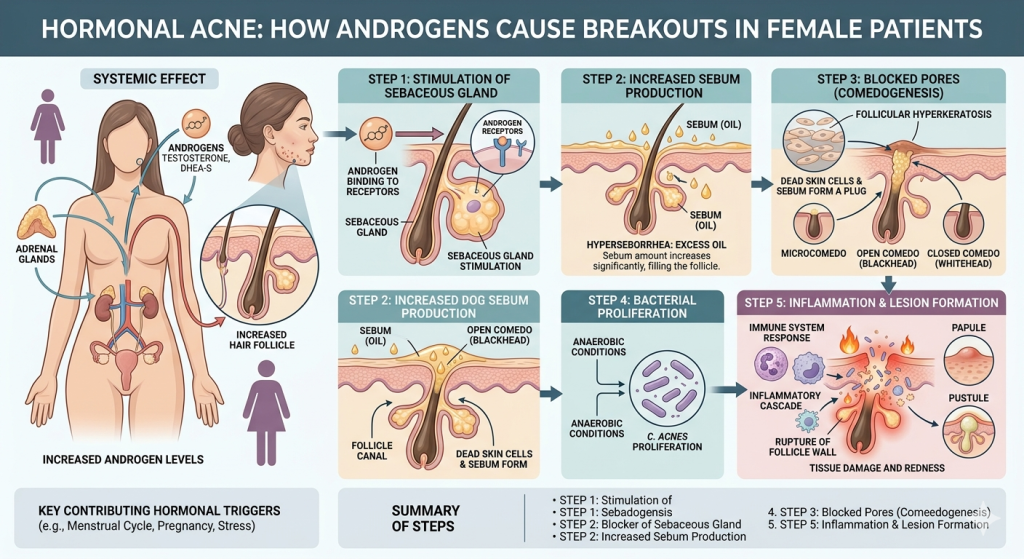
Treatment options for hormonal acne
1. Topical treatments
For many people, first-line treatment starts with topical medication rather than harsh scrubs or trendy routines. NICE recommends evidence-based options such as benzoyl peroxide, topical retinoids, azelaic acid, and combination products depending on acne severity. The NHS also notes that azelaic acid can help reduce dead skin and bacteria, and may be useful when other treatments are irritating. (NICE)
These treatments usually need time. NICE guidance commonly uses a 12-week treatment course before judging response, which matters because many people stop too early and assume nothing is working. (NICE)
2. Hormonal treatment
For women with clearly hormone-linked acne, hormonal treatment may help. The NHS states that the combined oral contraceptive pill can improve acne in women, especially when breakouts flare around periods or occur alongside hormonal conditions such as PCOS. Benefits can take months to become fully clear. (nhs.uk)
In specialist or clinician-guided care, anti-androgen treatment may also be considered for selected patients. Reviews in NIH sources explain that hormonal therapies target the androgen-sebum pathway, which is why they can be helpful when acne is driven by androgen activity. (PMC)
3. Oral antibiotics and isotretinoin
When acne is widespread, inflamed, or at risk of scarring, clinicians may recommend oral antibiotics in addition to topical treatment. NICE advises against antibiotic use alone because combination treatment is more appropriate and helps reduce concerns about resistance. For severe, scarring, or treatment-resistant acne, isotretinoin may be considered by specialists. (NICE)
4. Pregnancy considerations
Treatment choices change in pregnancy and when trying to conceive. NICE states that topical retinoids and oral tetracyclines are contraindicated during pregnancy and when planning a pregnancy. NHS guidance says benzoyl peroxide can be used during pregnancy because only a small amount is absorbed through the skin. (NICE)
5. Practical skin-aware strategies
A supportive routine usually works better than an aggressive one. Use a gentle cleanser, avoid over-scrubbing, choose non-comedogenic products where possible, and be consistent with prescribed treatment. Try not to pick or squeeze spots, especially deep ones, as this increases the risk of inflammation and scarring. If you suspect a cycle pattern, tracking breakouts alongside periods can be useful when speaking with a GP or dermatologist. NICE also highlights the importance of information, support, and skin-care advice in acne management. (NICE)
Common myths and misconceptions
One myth is that acne means your skin is dirty. It does not. Acne is a medical skin condition characterised by oil production, follicle blockage, inflammation, and changes in the microbiome. (NCBI)
Another myth is that hormonal acne only affects teenagers. In reality, adult female acne is common enough to be well described in both NHS information and medical literature. (nhs.uk)
A third myth is that you should dry acne out with harsh products. In practice, irritation can make skin harder to manage, which is why evidence-based, tolerable treatment plans matter. (nhs.uk)

When to seek medical advice
Please seek medical advice if acne is painful, widespread, leaving scars, affecting your confidence or mental well-being, not improving with pharmacy treatment, or if you have symptoms that suggest a hormonal condition, such as irregular periods, hirsutism, or fertility concerns. NICE also stresses the importance of considering the psychological impact of acne, not just the skin lesions themselves. (NICE)
FAQs
What causes hormonal acne?
Hormonal acne is mainly driven by androgen effects on the oil glands, which increase sebum production and contribute to blocked pores and inflammation. (PMC)
Does hormonal acne always mean I have PCOS?
No. PCOS is one possible cause, but many women have hormone-sensitive acne without PCOS. (nhs.uk)
Where does hormonal acne usually appear?
It often affects the lower face, chin, and jawline, though acne can also affect the chest, shoulders, and back. (nhs.uk)
Can birth control help hormonal acne?
Sometimes. The NHS says the combined oral contraceptive pill can help some women, particularly when acne flares around periods. (nhs.uk)
How long do treatments take to work?
Many acne treatments take about 12 weeks to assess the response properly. (NICE)
Can diet cause hormonal acne?
Diet is not the only cause, but some evidence suggests high-glycaemic dietary patterns may worsen acne in certain people. (PMC)
Is hormonal acne common in adulthood?
Yes. Adult acne, especially in women, is well recognised. (nhs.uk)
What acne treatments are unsafe in pregnancy?
NICE advises that topical retinoids and oral tetracyclines are contraindicated in pregnancy and when planning pregnancy. (NICE)
Medical disclaimer
This article is for educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Acne can overlap with other skin conditions and hormonal disorders, so please speak with a GP, pharmacist, dermatologist, or other qualified clinician for personalised care, especially if symptoms are severe, persistent, scarring, or linked with menstrual or fertility concerns.