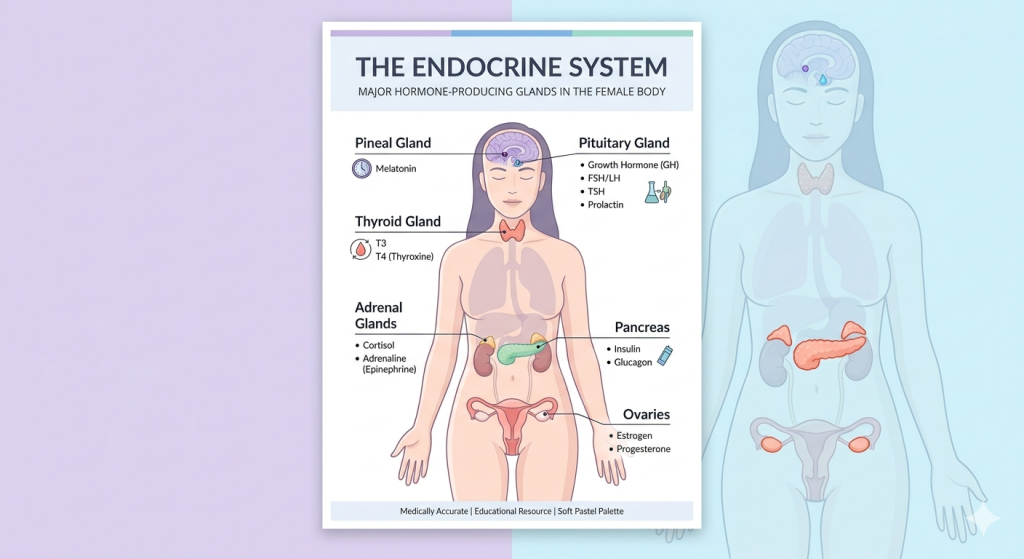
PCOS Symptoms
If you have been noticing PCOS symptoms like irregular periods, acne that will not settle, extra facial hair, or difficulty getting pregnant, it is understandable to feel confused or even brushed off. A lot of us are told these changes are “just hormones,” but sometimes they point to something more specific. PCOS symptoms can show up slowly, and they do not always look the same from one woman to another. In this guide, we will walk through what PCOS is, why it happens, the early signs to watch for, how diagnosis works, which treatments may help, and when it is time to get checked. (nhs.uk)
What is it?
Polycystic ovary syndrome, usually called PCOS, is a common hormone-related condition that affects ovulation, periods, skin, hair, fertility, and metabolic health. International guideline resources describe it as affecting around one in eight women, which helps explain why so many women experience PCOS symptoms at some point, even if the diagnosis is delayed. (Monash University)
Despite the name, PCOS is not just about ovarian cysts. In fact, you can have PCOS without having cysts seen on an ultrasound. Diagnosis is usually based on a pattern of symptoms and tests, not on a single scan result. (Office on Women’s Health)
What PCOS often affects
- Ovulation and menstrual cycles
- Hormone balance, especially androgen levels
- Skin and hair
- Fertility
- Blood sugar regulation and insulin response
- Longer-term health risks, such as type 2 diabetes and heart health concerns (Office on Women’s Health)
Why does it happen?
The exact cause of PCOS is not fully known, but it is strongly linked to hormone imbalance, insulin resistance, and family history. Many women with PCOS have bodies that do not respond well to insulin, so the body produces more of it. Higher insulin levels can push the ovaries to make more androgens, such as testosterone. That can disrupt normal ovulation and contribute to PCOS symptoms like irregular periods, acne, scalp hair thinning, and unwanted hair growth. (nhs.uk)
The hormone pattern behind PCOS
PCOS often involves a mix of:
- Irregular or absent ovulation
- Higher androgen activity
- Insulin resistance in many, though not all, women
- A tendency to run in families (nhs.uk)
Why symptoms can look different in different women
Some women mainly notice period problems. Others notice acne, hair changes, or trouble conceiving first. Some are in a smaller body and still have significant PCOS symptoms. Others notice symptoms becoming more obvious with weight gain or worsening insulin resistance. That is one reason PCOS can be missed for years. (Office on Women’s Health)

Evidence-Based Solutions
There is no single cure for PCOS, but there are evidence-based ways to manage it safely and effectively. The right plan depends on what matters most right now: cycle control, acne, hair growth, fertility, weight changes, or metabolic health. (Office on Women’s Health)
A. Medical interventions
i. Hormonal contraception
For women who are not trying to conceive, hormonal birth control is commonly used to make periods more regular, protect the womb lining, and sometimes improve acne and excess hair growth. (Office on Women’s Health)
ii. Metformin
Metformin is mainly a diabetes medicine, but it is also used for some women with PCOS, particularly where insulin resistance, prediabetes, or irregular ovulation are part of the picture. It may help some women ovulate more regularly. (Office on Women’s Health)
iii. Anti-androgen treatment
Some clinicians may use anti-androgen medicines to help with unwanted hair growth, acne, or scalp hair thinning. These are not suitable for everyone and need proper medical supervision, especially if pregnancy is possible. (Office on Women’s Health)
iv. Fertility treatment
If pregnancy is your goal, treatment may focus on helping ovulation happen more regularly. That may include ovulation-induction medicines and referral to a fertility specialist when needed. (Office on Women’s Health)
v. Practical note
The best treatment is not always the most aggressive one. Often, the most effective plan is the one that aligns with your symptoms, goals, and overall health risk profile.

Signs or symptoms
This is usually the section most women are searching for. PCOS symptoms often begin in the late teens or early 20s, but they can be recognised later too. (nhs.uk)
i. Common early signs of PCOS
- Irregular periods
- No periods for months at a time
- Difficulty getting pregnant because ovulation is irregular or absent
- Acne, especially if it is persistent or hard to treat
- Extra facial or body hair
- Hair thinning on the scalp
- Weight gain or difficulty managing weight
- Dark, velvety skin patches, often around the neck, groin, or underarms, which can be linked to insulin resistance (nhs.uk)
ii. Less obvious symptoms
Some women also notice:
- Oily skin
- Skin tags
- Mood changes or distress related to symptoms
- Snoring or poor sleep, if weight and insulin resistance are also issues
- Blood sugar concerns over time (NICHD)
iii. How PCOS is diagnosed
There is no single test for PCOS. Diagnosis usually involves a medical history, a symptom review, an examination, blood tests, and, sometimes, an ultrasound. A woman may be diagnosed if at least two of these are present after other causes are ruled out:
- Irregular or infrequent periods
- Signs or blood-test evidence of high androgen levels
- Polycystic ovaries on ultrasound (Office on Women’s Health)
iv. Tests your doctor may order
- Hormone blood tests
- Thyroid or other hormone tests to rule out similar conditions.
- Blood sugar or diabetes screening
- Cholesterol testing
- Pelvic ultrasound in some cases (Office on Women’s Health)
What is normal and when to pay attention
This part matters because not every uneven cycle means PCOS.
i. What can be normal
A normal adult menstrual cycle is typically 24 to 38 days, and small variations can occur from time to time. Periods can also be naturally less regular in the first few years after puberty and when approaching menopause. (Right Decisions)
ii. When it is worth paying attention
It is worth getting checked if:
- Your periods are usually more than 35 to 38 days apart.
- You skip periods for months.
- You have fewer than about 3 to 4 periods a year.
- You have persistent acne, facial hair growth, or scalp hair thinning.
- You are trying to conceive, and your cycles are very irregular.
- You notice dark patches of skin or symptoms that suggest insulin resistance (nhs.uk)
iii. Why regular checks matter
Long gaps between periods can mean the womb lining is not being shed regularly. Over time, this can increase the risk of endometrial thickening and, in some cases, endometrial cancer. That is one reason ongoing irregular bleeding should not be ignored. (Office on Women’s Health)

Holistic/Lifestyle Changes
Lifestyle changes are not a “quick fix,” and they are not about blame. They are simply part of good PCOS care, especially when insulin resistance is involved.
i. Nutrition
A balanced eating pattern that supports stable blood sugar can help many women with PCOS symptoms. That often means:
- Regular meals rather than long gaps
- High-fibre foods
- Protein with meals
- Fewer ultra-processed foods
- A sustainable approach rather than strict dieting
There is no single “PCOS diet” that works for everyone, but steady habits often matter more than perfection. (Office on Women’s Health)
ii. Physical activity
Regular movement can improve insulin sensitivity, support mood, and support cycle and metabolic health. It does not have to be extreme to be helpful. (Office on Women’s Health)
iii. Weight management, if relevant
For women who are overweight, even a modest reduction in body weight may improve cycle regularity and fertility. The goal is health support, not shame. Not every woman with PCOS needs weight loss advice, and PCOS can affect women of all body sizes. (Office on Women’s Health)
iv. Stress and sleep
Poor sleep and high stress do not cause PCOS on their own, but they can make symptoms harder to manage. Gentle routines, better sleep habits, and support for mental well-being can make a real difference in how manageable symptoms feel day to day. (NICHD)
v. Supplements
Some women ask about supplements for PCOS symptoms. Supplements may be discussed with a clinician, but they should not replace diagnosis or evidence-based care. It is safest to check before starting anything regularly, especially if you are trying to conceive or taking other medicines.
When to See a Doctor
This is the part we never want to leave vague.
See a doctor or doctor if:
- Your periods are very irregular, absent, or suddenly change
- You have new or worsening facial hair, acne, or scalp hair loss
- You have been trying to get pregnant, and your cycles are irregular
- You have symptoms of high blood sugar, such as unusual thirst or frequent urination
- You have dark, velvety skin patches
- You are gaining weight rapidly without a clear reason
- Your symptoms are affecting your mood, confidence, or quality of life (nhs.uk)
Seek urgent medical advice if:
- You have very heavy bleeding
- Severe pelvic pain
- Bleeding after sex, between periods, or after menopause
- Signs of pregnancy complications or severe illness

Key takeaway
PCOS symptoms can start quietly and feel easy to dismiss, especially when they show up as “just irregular periods” or “just bad skin.” But if your cycle is repeatedly off, you are skipping periods, or you are noticing hair, skin, or fertility changes, it is worth getting checked. A diagnosis does not mean something is “wrong” with you. It means you have more clarity, safer treatment options, and a better chance of protecting your long-term health. (Office on Women’s Health)
Frequently Asked Questions
Q: Can you have PCOS symptoms without cysts on your ovaries?
A: Yes. You do not need to have cysts on an ultrasound to have PCOS. Diagnosis can be made using other criteria, such as irregular periods and signs of higher androgen levels. (nhs.uk)
Q: What are the first PCOS symptoms most women notice?
Irregular periods, acne, facial hair growth, scalp hair thinning, and difficulty getting pregnant are among the most common early PCOS symptoms. (nhs.uk)
Q: Can PCOS symptoms start later in life?
Yes. Some women notice symptoms in their teens, while others are only diagnosed in their 20s, 30s, or when trying to conceive. (nhs.uk)
Q: Does having irregular periods always mean PCOS?
No. Irregular periods can happen for many reasons, including thyroid problems, stress, weight changes, perimenopause, and other hormone conditions. That is why proper assessment matters. (Office on Women’s Health)
Q: Can PCOS make it hard to get pregnant?
Yes. PCOS is one of the most common causes of female infertility because ovulation may happen irregularly or not at all. Many women still get pregnant with the right support and treatment. (nhs.uk)
Q: Is PCOS linked to diabetes?
A: Yes. PCOS is linked with insulin resistance, and it raises the risk of prediabetes and type 2 diabetes. (CDC)
Q: What should I ask my doctor if I think I have PCOS?
A: You can ask what tests are needed, whether your symptoms fit PCOS, whether other causes need ruling out, whether your womb lining needs protecting if you rarely bleed, and what treatment makes sense for your goals right now.
Medical disclaimer
This article is for education only and does not replace personal medical advice, diagnosis, or treatment. If you have concerning symptoms, missed periods, fertility concerns, unusual bleeding, or worsening pain, please speak to a qualified doctor, doctor, or gynaecology professional for individual assessment.