Can You Be Pregnant and Still Have Spotting? What It Means and When to Get Checked
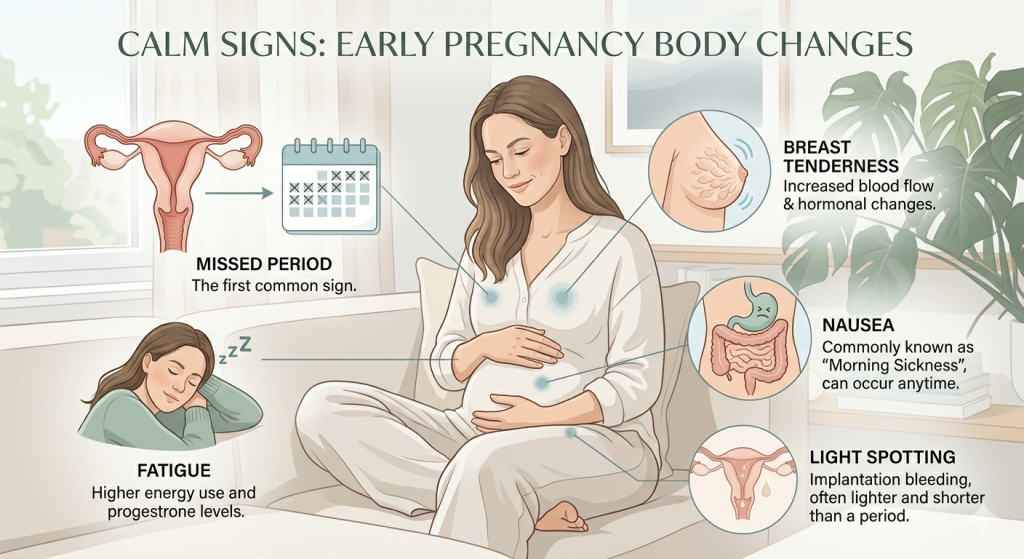
It can be unsettling to see spotting and immediately wonder, Could I still be pregnant? For many women, that small amount of pink, brown, or light red blood can bring a lot of worry, especially if a pregnancy test is positive or a period is late. The reassuring part is that yes, you can be pregnant and still have spotting. Light spotting can occur in early pregnancy and does not always indicate a problem. But because spotting can also happen with miscarriage, ectopic pregnancy, or other problems, it is worth paying attention to what the bleeding looks like and whether you have other symptoms. (ACOG) Quick answer Yes, it is possible to be pregnant and still have spotting. In early pregnancy, light spotting is fairly common and may happen for reasons such as implantation, cervical changes, or irritation after sex. But any bleeding in pregnancy should be taken seriously enough to monitor, and urgent help is needed if it is heavy, painful, or comes with dizziness, shoulder pain, fever, or fainting. (ACOG) What Does Implantation Bleeding Look Like? What is it? Spotting is a small amount of bleeding lighter than a period. It may show up as: a few drops of pink, red, or brown blood light marks on underwear blood only when wiping bleeding that does not soak a pad The NHS explains that spotting is different from heavier bleeding that needs a pad or soaks through one. In pregnancy, spotting can happen early on and may come and go. (nhs.uk) Why does it happen? There are a few reasons spotting can happen even when you are pregnant. Implantation bleeding Some women notice light spotting around the time a fertilised egg attaches to the uterine lining. This is often called implantation bleeding. It is usually light and short-lived, and it may happen around 10 to 14 days after conception. (Mayo Clinic) Changes to the cervix During pregnancy, the cervix has a richer blood supply and may bleed more easily. This can happen after sex, after a vaginal exam, or sometimes without a clear reason. Some NHS patient information also notes that the cervix can become softer and more likely to bleed a little. (Leeds Teaching Hospitals Flipbooks) A threatened miscarriage Sometimes spotting is the first sign that the pregnancy needs closer checking. Bleeding can happen with or without pain. Some pregnancies continue normally, while others do not, so that medical review may be needed depending on symptoms and timing. (ACOG) Ectopic pregnancy This is when a pregnancy develops outside the uterus, usually in a fallopian tube. It can cause spotting or bleeding, often with pain. This needs urgent medical attention. (CKS) Other causes Bleeding later in pregnancy can have other explanations, and later bleeding is more likely to need urgent assessment. Light bloody mucus near the end of pregnancy may also be part of the “bloody show” as labour approaches. (Mayo Clinic) Ectopic Pregnancy Signs: When to Get Help Signs or symptoms Spotting in pregnancy is more likely to be mild when it is: light pink, brown, or small amounts of red blood brief not getting heavier not linked with strong cramping or pain Symptoms that matter just as much as the spotting itself include: lower tummy or pelvic pain cramping shoulder tip pain dizziness or feeling faint fever or chills passing clots or tissue bleeding that becomes heavier than spotting These extra symptoms can help indicate whether the cause is less serious or whether you need urgent review. (Mayo Clinic) What is normal, and when to pay attention Light spotting in early pregnancy can be common. ACOG says bleeding in early pregnancy is common, and Mayo Clinic notes that light spotting that goes away quickly may need mentioning at your next prenatal visit. (ACOG) Even so, it is wise not to ignore it. Spotting may be less concerning when it is: very light short-lived not associated with pain not becoming heavier Pay closer attention if: it lasts more than a day it becomes bright red or heavier you need a pad you develop cramps, pelvic pain, or back pain you feel faint, weak, or unwell Mayo Clinic advises contacting a healthcare professional within 24 hours if bleeding lasts longer than a day, and right away if bleeding is moderate to heavy or accompanied by pain, fever, chills, or tissue passage. (Mayo Clinic) A practical reminder: if you think you may be pregnant and notice spotting, take a pregnancy test if you have not already, note the colour and amount of blood, and keep track of any pain or new symptoms. That information can be helpful if you need medical advice. Early Pregnancy Symptoms Before a Missed Period When to speak to a doctor Speak to a doctor, midwife, early pregnancy unit, or urgent care service if you are pregnant or think you might be pregnant and have spotting. Get medical help urgently if you have: one-sided pelvic or abdominal pain shoulder tip pain fainting or severe dizziness heavy bleeding severe cramps fever passage of clots or tissue These can be warning signs of miscarriage or ectopic pregnancy, both of which need prompt assessment. NHS guidance also advises contacting maternity or medical services if bleeding happens during pregnancy, because even when it turns out to be minor, it is safer to get checked. (nhs.uk) Key takeaway Yes, you can be pregnant and still have spotting. Light spotting in early pregnancy is not unusual and can happen for reasons that are not harmful, including implantation or cervical changes. But spotting should never be dismissed completely, because sometimes it is an early sign that the pregnancy needs medical assessment. The safest approach is to stay observant, monitor your symptoms, and seek prompt help if the bleeding is heavy, painful, or paired with anything that feels off. (ACOG) FAQs Can you still be pregnant if you have light bleeding? Yes. Light bleeding or spotting can happen in pregnancy, especially early on. It does not always mean the pregnancy has ended, but
Can You Be Pregnant and Still Have Spotting? What It Means and When to Get Checked Read More »