Introduction
Have you ever looked at a cluster of symptoms and thought, What is going on with my body?
Maybe your periods have changed, your sleep is worse, your mood feels less steady, your skin is breaking out, or you feel tired in a way that does not quite make sense. For many women, especially over 45, that question quickly becomes: Are my hormones out of balance?
It is a very common thought, and it is not unreasonable. Hormones influence menstrual cycles, ovulation, metabolism, temperature regulation, mood, fertility, and more. But “hormonal imbalance” is not a single diagnosis. It is a broad phrase people often use when one or more hormones are too high, too low, or fluctuating in a way that affects how they feel. That can happen for many reasons, from normal life-stage changes to conditions such as PCOS or thyroid disease.
In brief
Hormonal imbalance in women can be caused by normal reproductive transitions such as perimenopause and menopause, by conditions that affect ovulation or androgens such as PCOS, by thyroid problems, by pregnancy and postpartum hormonal shifts, by raised prolactin, and sometimes by medicines including hormonal contraception. The exact cause depends on which hormones are involved and what pattern of symptoms you are noticing. Ongoing changes in periods, sleep, energy, skin, hair, temperature tolerance, or fertility are worth paying attention to, especially if they are persistent or getting worse.
PCOS Symptoms: What Irregular Periods May Be Telling You
Quick answer
A hormonal imbalance occurs when hormones are not at the levels or in the patterns your body needs for its usual rhythm. In women over 45, one of the most common reasons is the natural shift toward perimenopause, but that is far from the only cause. Thyroid disorders, PCOS, pregnancy and postpartum changes, and other endocrine issues can all create symptoms that feel hormonal. The most helpful next step is not to guess mindlessly, but to look at the pattern of symptoms, your age and life stage, and whether the changes are disrupting daily life.
Table of contents
- What is a hormonal imbalance?
- Why does it happen?
- How hormones or body systems are involved
- Common signs, symptoms, or patterns
- Common causes, triggers, or risk factors
- How age, lifestyle, stress, or health conditions may affect it
- What can help or what to do next
- When to speak to a doctor
- Common myths or misunderstandings
- Key takeaway
- FAQs
What is a hormonal imbalance?
Hormones are chemical messengers made by glands in the endocrine system. They travel through the bloodstream and help regulate many core body functions, including metabolism, sexual function, reproduction, growth, and mood. Because hormones affect so many systems, even a relatively small change can sometimes show up in noticeable ways.
When people say “hormonal imbalance,” they often mean that hormone levels are too high, too low, or fluctuating differently than expected for their body and life stage. In practice, this can involve oestrogen, progesterone, androgens such as testosterone, thyroid hormones, insulin-related pathways, prolactin, or a mix of these. The phrase is useful as a starting point, but it is not a final explanation on its own.
That is why two women can both say, “My hormones feel off,” while having very different underlying reasons. One may be entering perimenopause. Another may have thyroid disease. Another may be dealing with PCOS or postpartum hormone shifts. The body can feel similarly unsettled for different biological reasons.
Why does it happen?
Hormonal imbalance happens because the endocrine system works like a communication network. The brain, ovaries, thyroid, adrenal glands, pancreas, and other organs constantly send and respond to signals. If one part of that signalling system changes, other parts can be affected too.
In women over 45, one major reason is age-related reproductive change. During perimenopause, the ovaries start making different amounts of oestrogen and progesterone than usual, and those changes can be unpredictable. This is why symptoms may seem to arrive in waves rather than in a neat, orderly pattern.
But age is not the whole story. Ovulation problems, thyroid dysfunction, androgen-related conditions, autoimmune disease, and pregnancy-related endocrine shifts can all change how the body feels. In some cases, symptoms reflect a true hormone disorder. In others, they reflect a normal transition that still deserves support and clear information.
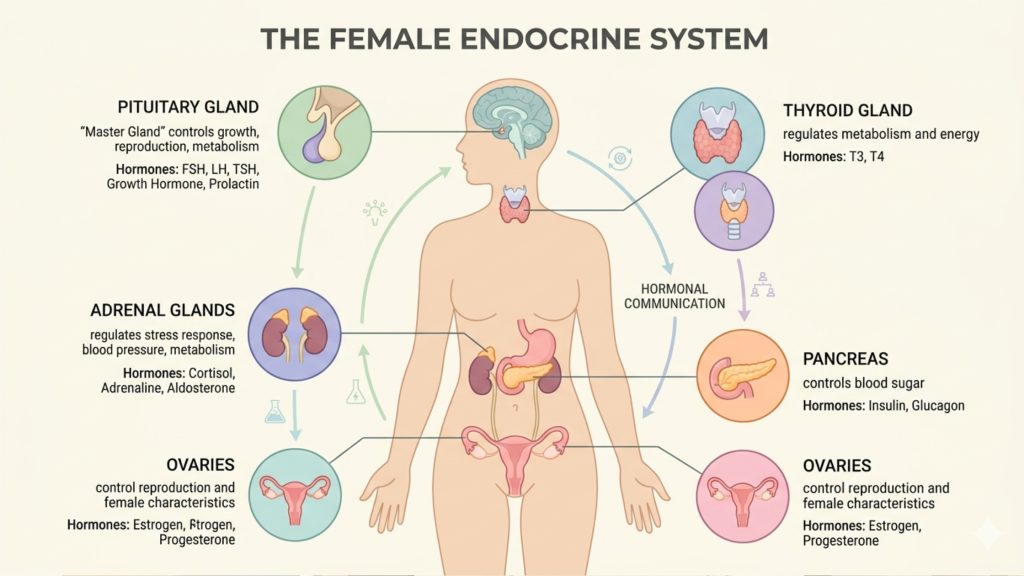
How hormones or body systems are involved
i. Ovaries and reproductive hormones
The ovaries help regulate oestrogen and progesterone, which influence the menstrual cycle, ovulation, vaginal tissues, bone health, and more. As ovarian function shifts, periods may become more or less regular, bleeding patterns can change, and symptoms such as sleep disruption, hot flushes, or mood changes may appear. This is especially relevant in perimenopause and menopause.
ii. Thyroid hormones
Thyroid hormones help regulate metabolism and affect many organs. When thyroid hormone is too low, the body tends to slow down, which can lead to fatigue, weight gain, feeling cold, dry skin, hair thinning, and heavy or irregular periods. When thyroid hormone is too high, body systems can feel sped up.
iii. Androgens
Androgens are often thought of as “male” hormones, but women make them too. If androgen levels rise, or if the body becomes more sensitive to them, symptoms can include acne, facial or body hair growth, and scalp hair thinning. NHS guidance notes that this kind of pattern is common in PCOS and can also show up with hirsutism.
iv. Prolactin and other signalling hormones
Prolactin is best known for its role in milk production, but when elevated outside its usual context, it can interfere with ovulation and menstrual cycles. Hormones such as FSH also play a role in ovarian signalling, which is why hormone interpretation is often more complex than a single number on a test result.
Common Menopause Symptoms and Why They Happen
Common signs, symptoms, or patterns
Hormonal changes do not look the same in everyone, but some patterns commonly make women wonder if hormones are involved.
You might notice:
- Irregular periods or missed periods
- heavier or lighter bleeding than usual
- difficulty getting pregnant
- acne or oilier skin
- increased facial or body hair
- thinning hair or hair loss from the scalp
- hot flushes or night sweats
- sleep problems
- fatigue
- mood changes
- lower sex drive
- weight changes
- feeling unusually cold or unusually hot
- vaginal dryness in some life stages
Symptoms often come in clusters. For example, irregular periods, acne, and unwanted hair growth may suggest an androgen-related pattern such as PCOS. Heavy periods, fatigue, feeling cold, and dry, thinning hair may be better explained by hypothyroidism. Hot flushes, unpredictable cycles, and sleep disturbance in a woman over 45 may point toward perimenopause. Looking at the combination is often more useful than focusing on one symptom in isolation.
Common causes, triggers, or risk factors
1. Perimenopause and menopause
For women above 45, this is one of the biggest causes of feeling hormonally “off.” During the transition to menopause, hormone levels may change randomly, and the ovaries produce different amounts of oestrogen and progesterone than usual. This can cause irregular periods, sleep problems, mood shifts, night sweats, and hot flushes.
2. PCOS
PCOS is a common hormone-related condition that can affect ovulation and androgen levels. NHS guidance lists symptoms such as irregular or absent periods, difficulty getting pregnant, excess hair growth, weight gain, thinning scalp hair, oily skin, and acne. Some women are diagnosed younger, but symptoms and fertility concerns can continue well into their late 30s and 40s.
3. Thyroid disease
Thyroid problems are a major and sometimes overlooked cause of hormone-related symptoms in women. Hypothyroidism can cause fatigue, weight gain, cold intolerance, dry skin, dry or thinning hair, heavy or irregular periods, and fertility problems. Hashimoto’s disease, a common autoimmune cause of hypothyroidism, is much more common in women and often appears between ages 30 and 50.
4. Pregnancy and postpartum hormone shifts
Pregnancy causes profound hormonal changes, and the period after birth does too. Some postpartum symptoms overlap with normal recovery, but thyroid-related issues can also appear after pregnancy. NIDDK notes that hypothyroid symptoms in the first months after birth may sometimes be mistaken for “baby blues” or general exhaustion.
5. Hormonal contraception or medicines
Some hormonal birth control methods can change bleeding patterns or lead to spotting, especially in the early months. This does not always mean something is wrong, but it can make women feel as though their hormones have suddenly shifted. Other medicines may also affect the endocrine system depending on the situation.
6. Raised prolactin or other endocrine disorders
Higher prolactin levels can affect menstrual cycles, ovulation, and fertility. Less commonly, other endocrine disorders may also play a role, which is one reason persistent symptoms deserve proper assessment rather than a broad assumption.
How age, lifestyle, stress, or health conditions may affect it
Age matters because hormones do not stay static. In the years leading up to menopause, hormone patterns become less predictable. That unpredictability itself can feel unsettling. A woman may still have periods, but they may be closer together, farther apart, heavier or lighter, or accompanied by new sleep or temperature symptoms.
Lifestyle matters too, though it is important not to reduce everything to stress or self-care. Poor sleep, high ongoing stress, and daily strain can worsen how symptoms feel, especially if sleep is already being disrupted by perimenopause or another hormone-related issue. Stress may not be the root cause, but it can make existing problems harder to cope with. This is partly why the same hormone shift can feel manageable for one woman and overwhelming for another.
Health conditions are also important. Autoimmune thyroid disease is one example. NIDDK notes that Hashimoto’s disease is 4 to 10 times more common in women than in men, and the risk is higher if there is a family history of or other autoimmune disease. Existing reproductive, metabolic, or endocrine conditions can shape both symptoms and risk.
Weight changes can also interact with hormone symptoms, especially around menopause and in conditions like PCOS. Office on Women’s Health notes that low oestrogen and age-related changes, such as gaining weight, can affect health risks during menopause. This does not mean weight is the sole cause, but it can be part of the picture.
What can help or what to do next
The most helpful first step is usually not a dramatic detox, cleanse, or panic-driven supplement routine. It is getting clearer about the pattern.
Try this:
- track your periods, bleeding changes, sleep, mood, skin changes, hot flushes, headaches, and energy for at least a few weeks
- Note your age, contraception, medicines, and whether you may be in a life stage such as postpartum or perimenopause.
- Watch for clusters rather than a single symptom.
- pay attention to how much symptoms affect work, sleep, relationships, or daily life
- Book a medical review if the pattern is new, worsening, or ongoing.
A practical reminder: hormone testing can be useful, but it is not always straightforward. Some hormones naturally fluctuate through the menstrual cycle, and results need to be interpreted alongside symptoms, cycle timing, age, and medical history. A normal-looking result does not always cancel out a real symptom pattern, and an abnormal result still needs context.
What helps next depends on the cause. For PCOS, symptom management and fertility planning matter most. For thyroid disease, proper diagnosis and treatment can make a major difference. For perimenopause, lifestyle support, symptom tracking, and sometimes medical treatment may be appropriate. There is no one-size-fits-all answer because the cause shapes the right plan.

When to speak to a doctor
Speak to a doctor or qualified healthcare professional if:
- your periods have become very irregular, very heavy, or have stopped unexpectedly
- You are having trouble getting pregnant
- You have new, unwanted facial hair, persistent acne, or scalp hair thinning
- You have ongoing fatigue, weight change, feeling cold, or other possible thyroid-type symptoms
- you are getting hot flushes, night sweats, or sleep problems that affect daily life
- Your symptoms are persistent, worsening, or do not feel normal for you
Seek urgent help if bleeding is very heavy, you feel faint, or you have severe or sudden symptoms. While many hormone-related changes are not emergencies, extreme bleeding or major physical deterioration should not be watched passively. This article is educational and cannot replace a personal medical assessment.
Common myths or misunderstandings
Myth 1: “Hormonal imbalance” is a diagnosis by itself
Not really. It is a broad description. The real question is which hormones are involved and why.
Myth 2: Every symptom in your late 30s or 40s is just menopause
Perimenopause is common, but it is not the answer to everything. Thyroid disease, PCOS, medication effects, and other conditions can overlap.
Myth 3: If symptoms are hormonal, a single blood test will explain everything
Hormone interpretation is often more nuanced than that because some hormones change with the cycle or life stage. Clinical context matters.
Myth 4: Stress is always the real cause
Stress can worsen symptoms, but it should not be used to dismiss persistent bleeding changes, fertility problems, or possible thyroid symptoms.
Myth 5: You should fix hormones with online advice before talking to a doctor
Some symptoms do improve with better sleep, nutrition, or support, but others need assessment and treatment. Self-diagnosis can delay the right help.
Key takeaway
The causes of hormonal imbalance in women are varied, and that is exactly why the phrase can feel confusing. For women over 35, perimenopause is a very common reason hormones seem to shift, but it is far from the only one. PCOS, thyroid disease, pregnancy or postpartum changes, raised prolactin, and medication effects can all play a role. The most useful approach is to notice the pattern, avoid jumping to conclusions, and get proper support when symptoms are persistent, disruptive, or unusual for you. A calm, informed next step is almost always more helpful than guesswork.
FAQs
What is the most common cause of hormonal imbalance in women over 45?
One of the most common causes is perimenopause, when oestrogen and progesterone levels start changing less predictably. But thyroid disease and PCOS are also common causes of hormone-related symptoms.
Can thyroid problems feel like a hormonal imbalance?
Yes. Thyroid hormones affect metabolism, energy, temperature tolerance, periods, hair, and fertility, so many women describe thyroid symptoms as feeling hormonally “off.”
Does PCOS only affect younger women?
No. PCOS is often noticed earlier in life, but its symptoms can continue well into the late 30s and 40s, especially around fertility, irregular cycles, acne, and hair changes.
Can stress cause a hormonal imbalance?
Stress can influence hormone pathways and worsen symptoms, especially sleep and mood symptoms, but it is not the only possible cause. Persistent period changes, fertility problems, or thyroid-like symptoms still deserve proper evaluation.
Why do my hormones feel suddenly out of balance?
Symptoms can feel sudden when several small changes arrive together, such as altered periods, acne, poor sleep, and mood changes. Common possibilities include perimenopause, thyroid changes, PCOS, pregnancy-related shifts, or medicine-related effects.
Can hormonal birth control make hormones feel off?
Yes, hormonal contraception can change bleeding patterns and sometimes create symptoms that feel like a hormonal shift, especially when starting or changing methods.
When should I worry about hormone symptoms?
You should speak to a clinician if symptoms are new, ongoing, worsening, affecting daily life, causing heavy or irregular bleeding, or interfering with fertility.


