Introduction
If you are searching for morning sickness relief in pregnancy, there is a good chance you are not just feeling a little queasy. You may be exhausted, put off by smells you used to ignore, struggling to eat, or wondering whether what you are feeling is still “normal.” Many of us grow up hearing the phrase morning sickness, but the reality is often much more disruptive, much less tidy, and not limited to the morning at all.
The good news is that morning sickness relief in pregnancy is possible, and there are practical, evidence-based ways to make symptoms more manageable. In this guide, we will walk through why nausea and vomiting occur in pregnancy, which symptoms are common, which treatments actually help, when medication may be appropriate, and when symptoms require medical attention. We will also cover the red flags that may point to hyperemesis gravidarum, the more severe end of the spectrum.
What is morning sickness?
Morning sickness is the common name for nausea and vomiting of pregnancy. Despite the name, it can happen at any time of day or night. It usually begins early, often between 4 and 7 weeks of pregnancy, and for many women it starts to improve by 16 to 20 weeks. It is extremely common, and mild to moderate symptoms are part of many healthy pregnancies. (RCOG)
Still, common does not mean easy. Morning sickness can affect appetite, sleep, work, mood, hydration, and day-to-day functioning. That is why honest, practical morning sickness relief in pregnancy matters so much.
Why does morning sickness happen?
Morning sickness is not caused by weakness, anxiety, or “doing pregnancy badly.” It is linked to the normal biological changes of early pregnancy.
One of the main drivers appears to be rising pregnancy hormones. The placenta produces hormones very early, and these seem to affect the stomach, appetite, and the brain’s nausea pathways. The Royal College of Obstetricians and Gynaecologists notes that pregnancy sickness is thought to be related to hormones, and research suggests that GDF-15, a hormone produced by the placenta, may play an important role in nausea and appetite loss. (RCOG)
Other factors may make symptoms more noticeable, too:
- A heightened sense of smell
- Slower stomach emptying
- Fatigue
- Hunger or long gaps without eating
- Carrying twins or higher-order multiples
- A personal history of severe pregnancy sickness
- A previous history of hyperemesis gravidarum (RCOG)
This is one reason morning sickness relief in pregnancy usually works best when we look at the whole picture: food, fluids, triggers, rest, and symptom severity.

Symptoms and signs
You may be experiencing:
- Persistent nausea, with or without vomiting
- Vomiting after meals
- Dry heaving or retching
- A strong aversion to smells, foods, or textures
- Feeling worse when your stomach is empty
- Loss of appetite
- Excess saliva
- Dizziness or weakness
- Trouble drinking enough fluids
- Fatigue from repeated nausea or vomiting
- Symptoms that last all day, not just in the morning
Some women mainly feel queasy. Others vomit several times a day. Both experiences can be distressing, and both deserve support.
What actually helps with morning sickness relief in pregnancy?
For many women, the most effective approach is not one miracle remedy but a combination of small, practical strategies.
a. Eat little and often
An empty stomach can make nausea worse. Small, frequent meals or snacks may be easier to tolerate than three large meals. NHS guidance suggests trying 6 small meals a day rather than larger meals. (nhs.uk)
Helpful choices often include:
- Dry toast
- Plain crackers or biscuits
- Plain rice or pasta
- Potatoes
- Cereal
- Banana
- Simple protein snacks you can tolerate
b. Drink in small, regular sips
Hydration matters, but big drinks can sometimes trigger vomiting. Small sips throughout the day work better than trying to drink a full glass at once. Water, ice chips, diluted juice, or oral rehydration drinks may be easier on the stomach. NHS advice emphasises the importance of staying hydrated, and the inability to keep fluids down is a warning sign that needs attention. (nhs.uk)
c. Keep bland foods nearby
Many women do better with bland, dry foods, especially before getting out of bed or during long gaps between meals. NHS advice includes foods such as plain biscuits, dry bread, toast, pasta, and jacket potatoes. (nhs.uk)
d. Avoid strong triggers
Common triggers include:
- Cooking smells
- Greasy or spicy food
- Hot rooms
- Fatigue
- Long car journeys
- Certain toothpaste flavours
- Strong perfumes
Trying colder foods may help because they often smell less intense.
e. Ginger may help
NICE recommends that women with mild to moderate nausea and vomiting who prefer a non-drug option can try ginger. NHS guidance also notes that some people find ginger helpful. (NICE)
You might try:
- Ginger tea
- Ginger biscuits
- Ginger chews
- Ginger ale made with real ginger
It is sensible to check with a pharmacist or maternity clinician before taking concentrated ginger supplements.
f. Acupressure may be worth trying
Acupressure wristbands are not a guaranteed fix, but some women do find them useful. NICE says acupressure can be considered as an adjunct treatment for moderate to severe nausea and vomiting, and NHS pregnancy guidance mentions wristbands as something some people find helpful. (NICE)
g. Rest matters more than it sounds
Exhaustion can intensify nausea. Rest will not “cure” pregnancy sickness, but being overtired often makes symptoms more difficult to tolerate. Where possible, lowering physical demands for a short period may help.
Medical interventions that may be used
Sometimes lifestyle changes are not enough. That is not failure. It simply means symptoms may need medical treatment.
NICE recommends offering an antiemetic to pregnant women who choose pharmacological treatment for nausea and vomiting in pregnancy, after discussing the benefits and drawbacks. (NICE)
a. Vitamin B6 and doxylamine
ACOG states that vitamin B6 (pyridoxine) is a safe over-the-counter option that may be tried first, and doxylamine may be added if needed; a prescription combination product is also available in some settings. (acog.org)
b. Prescription anti-sickness medicines
Depending on where you live, medicines commonly considered include:
- Doxylamine/pyridoxine
- Cyclizine
- Promethazine
- Metoclopramide
- Prochlorperazine
- Ondansetron
NICE’s treatment table notes that doxylamine/pyridoxine is the only product specifically licensed in the UK for nausea and vomiting in pregnancy. Metoclopramide is generally treated as a second-line option and is not recommended for more than 5 days because of the risk of neurological side effects. Ondansetron may be effective, but the NICE table advises discussing the small possible first-trimester risk signal, including a slight increase in the risk of cleft lip or palate, as part of shared decision-making. (NICE)
This is why morning sickness relief in pregnancy should never become a self-prescribing exercise. The right medicine depends on:
- How severe the symptoms are
- How far along is the pregnancy
- Whether dehydration is present
- Whether first-line treatment has already failed
- Your own medical history
c. IV fluids and hospital treatment
For moderate to severe symptoms, NICE recommends considering intravenous fluids, ideally as an outpatient where appropriate. If vomiting is severe and not responding to community treatment, inpatient care may be needed. (NICE)
This is especially important when morning sickness is progressing toward hyperemesis gravidarum.
When morning sickness may be more serious
There is a point at which ordinary pregnancy sickness stops being merely unpleasant and becomes medically significant.
The severe form is called hyperemesis gravidarum. RCOG states it can affect up to 3 in 100 pregnant women, and NHS guidance notes that severe vomiting can lead to dehydration and malnourishment. (RCOG)
Possible signs that symptoms are becoming more serious include:
- You cannot keep fluids down
- You are losing weight
- You are passing very little urine
- Urine is very dark
- You feel faint or dizzy when standing
- You are vomiting repeatedly throughout the day
- You feel too unwell to manage basic daily activities
This is where early assessment matters. Effective morning sickness relief in pregnancy is not only about comfort. It is also about preventing complications.
When to see a doctor
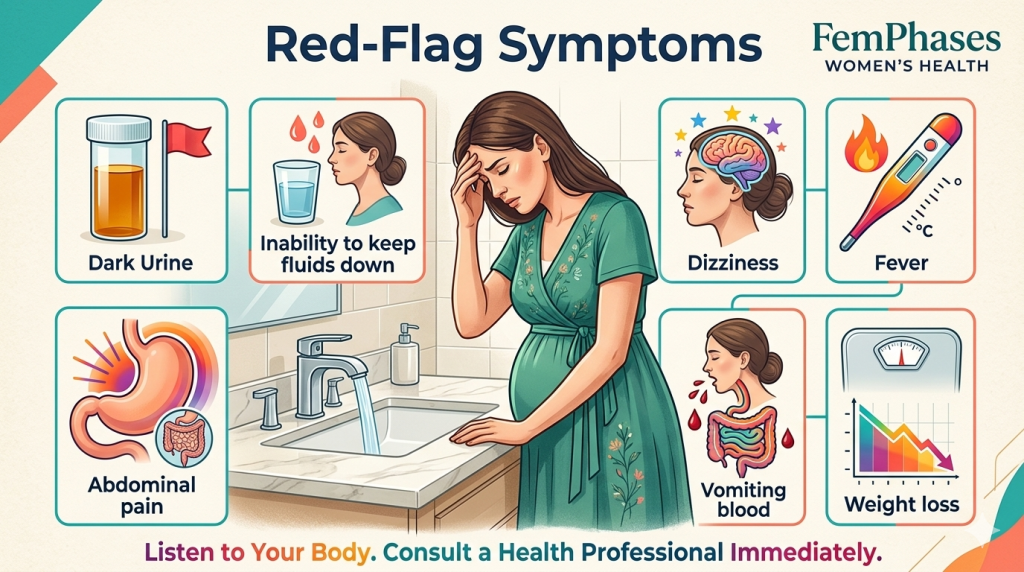
Please seek medical advice promptly if you have any of the following red flags:
- Very dark urine or no urine for more than 8 hours
- Inability to keep food or fluids down for 24 hours
- Feeling very weak, dizzy, or faint when standing
- Weight loss
- Abdominal pain
- High temperature
- Vomiting blood (nhs.uk)
Also, contact your midwife, GP, maternity unit, or urgent care service if:
- Symptoms are getting worse rather than better
- You cannot take prescribed medication because you vomit it back up
- You have signs of dehydration
- You are worried you may have hyperemesis gravidarum
- You are struggling emotionally because the symptoms are relentless
RCOG and NHS guidance both stress that severe symptoms deserve treatment and should not be dismissed. (RCOG)
Key takeaway
Morning sickness can be common yet deeply disruptive. Safe, practical morning sickness relief in pregnancy often begins with small meals, steady fluids, bland foods, rest, trigger avoidance, ginger, and sometimes acupressure. When symptoms go beyond mild to moderate, anti-sickness medication may be appropriate, and for severe symptoms, IV fluids or hospital care may be needed.
The most important message is this: you do not need to wait until you are severely unwell before asking for help. If you are struggling to drink, losing weight, feeling faint, or unable to function, please reach out early.
Frequently Asked Questions
Q: Is morning sickness a good sign in pregnancy?
Answer
Morning sickness is common in healthy pregnancies, but its presence or absence does not reliably measure how healthy a pregnancy is. Some women have significant nausea, some have almost none, and both can still have normal pregnancies.
Q: When does morning sickness usually start and stop?
Answer
It often starts between 4 and 7 weeks of pregnancy and, for many women, improves by 16 to 20 weeks. Some women have symptoms for longer. (RCOG)
Q: What is the best food for morning sickness relief in pregnancy?
Answer
There is no single best food, but many women tolerate small, bland, dry foods better than rich or strongly scented meals. Crackers, toast, plain biscuits, potatoes, pasta, and simple snacks often help.
Q: Can I take anti-sickness medicine while pregnant?
Answer
Sometimes, yes. Several antiemetics are used in pregnancy, but the best choice depends on your symptoms, gestation, and medical history. It is important to discuss this with your doctor, midwife, or pharmacist rather than choosing medication on your own. (NICE)
Q: How do I know if it is hyperemesis gravidarum?
Answer
Hyperemesis gravidarum is the severe end of pregnancy sickness and may involve persistent vomiting, dehydration, difficulty keeping fluids down, and weight loss. If you are passing very little urine, feel faint, or cannot keep fluids down, seek urgent medical advice. (nhs.uk)
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.








