Introduction: You Are Not the Only One!
The journey to parenthood is rarely a straight line. For many of us, the decision to start a family comes with a mixture of profound excitement and, quite often, a quiet, nagging anxiety. We live in a world where we are used to being in control, yet fertility can sometimes feel like a mysterious biological black box.
If you’ve been tracking your temperature, peeing on ovulation sticks, or simply wondering why it hasn’t happened yet, please know that your feelings are valid. We understand the unique emotional weight of the “two-week wait.” In this guide, we are going to strip away the myths and look at the clinical evidence.
You will learn how your hormones orchestrate the reproductive cycle, which lifestyle changes actually move the needle, and when it is time to seek professional medical guidance. Our goal is to empower you with clarity so you can navigate your fertility journey with confidence and peace of mind.
The “Why”: The Biological Dance of Conception
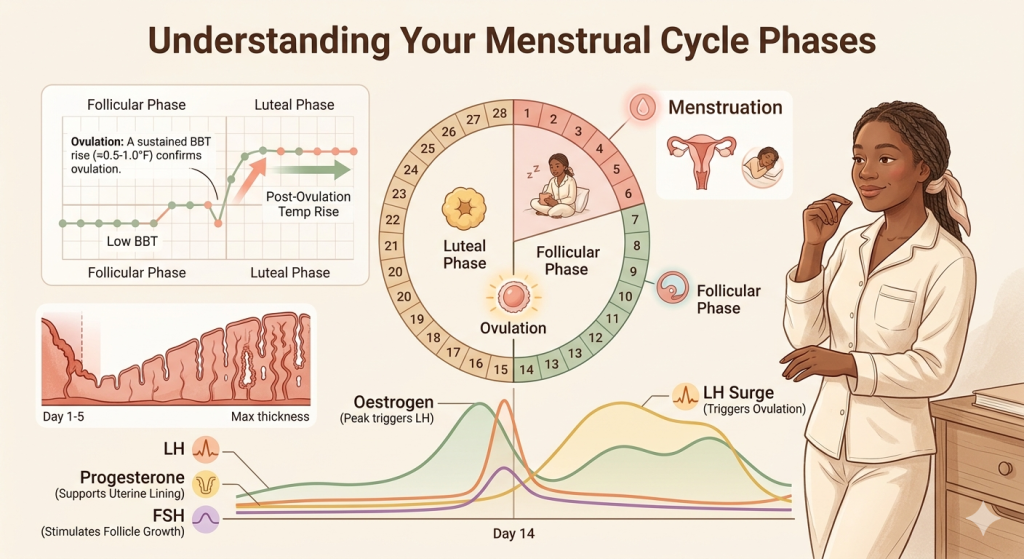
At its core, fertility is a high-stakes coordination between your brain and your ovaries. It starts in the hypothalamus, which signals the pituitary gland to release Follicle-Stimulating Hormone (FSH). This hormone acts like a starter pistol, telling your ovaries to grow a handful of follicles, each containing an egg.
As these follicles grow, they produce oestrogen, which thickens the lining of your uterus (the endometrium) to create a plush “nest.” Eventually, one dominant follicle wins the race, triggering a surge in Luteinizing Hormone (LH). This surge signals the release of the egg—this is ovulation.
Once the egg is released, the empty follicle transforms into the corpus luteum, which produces progesterone. Progesterone is the “pro-gestation” hormone; it stabilises the uterine lining. If sperm meets the egg in the fallopian tube, the resulting embryo travels to the uterus to implant. If not, hormone levels drop, the lining sheds, and the cycle begins anew. Understanding this rhythm is the first step in optimising your fertility.
Basal Body Temperature Tracking for Ovulation: How It Works and What It Can Tell You
The Symptoms and Signs: Listening to Your Body
Your body provides subtle clues every month that indicate your fertility status. Learning to read these “biomarkers” can significantly reduce the time to conception. Here is what you should be looking for:
- Cervical Mucus Changes: As you approach ovulation, your discharge will become clear, stretchy, and slippery, resembling raw egg whites. This protects sperm and helps them swim.
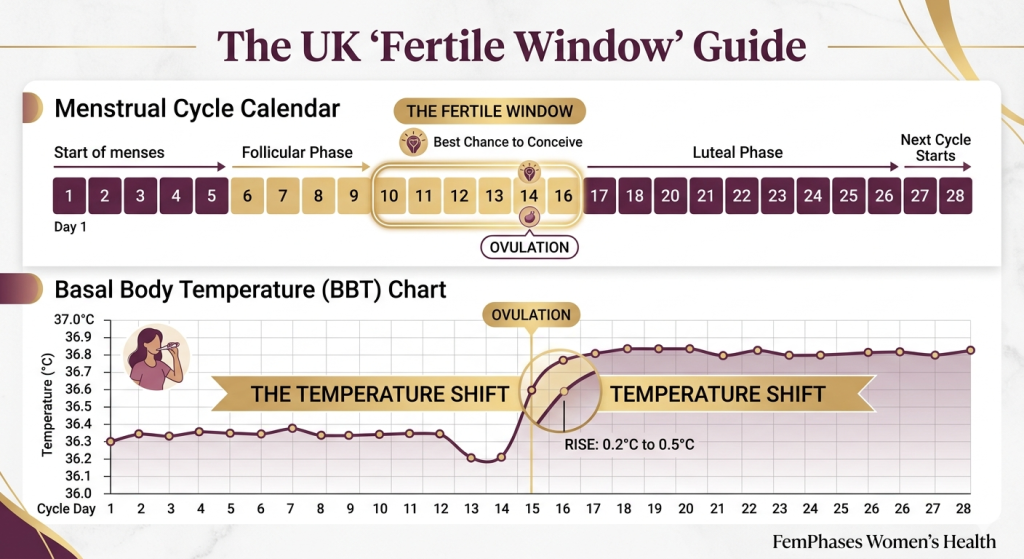
- Basal Body Temperature (BBT) Shift: A slight rise in your resting temperature (usually about 0.2°C to 0.5°C) occurs right after ovulation due to increased progesterone.
- Ovulation Pain (Mittelschmerz): Some women feel a dull ache or sharp twinge on one side of the lower abdomen mid-cycle.
- Breast Tenderness: Fluctuating hormones post-ovulation can make breast tissue feel heavy or sensitive.
- Increased Libido: Nature has a way of boosting your sex drive exactly when you are most fertile.
- Positive OPK: Ovulation Predictor Kits (OPKs) detect the LH surge in your urine 24–36 hours before the egg is released.
Evidence-Based Solutions: Lifestyle and Nutrition
While we cannot control every aspect of biology, we can certainly influence the “soil” in which the seed grows. Optimising your lifestyle is about reducing systemic inflammation and balancing the endocrine system to support peak fertility.
1. The Fertility Diet
Research, including the landmark “Fertility Diet” study from Harvard, suggests that nutrition plays a massive role in ovulatory function. Focus on:
- Complex Carbohydrates: Swap white bread and sugary cereals for whole grains like quinoa and oats to keep insulin stable. High insulin can disrupt ovulation.
- Plant-Based Proteins: Replacing one serving of meat per day with beans, lentils, or nuts has been shown to reduce the risk of ovulatory infertility.
- Full-Fat Dairy: Surprisingly, small amounts of full-fat yoghurt or milk are associated with better fertility outcomes than low-fat versions.
2. Targeted Supplementation
While a prenatal vitamin is the baseline, specific supplements can support egg quality:
- Folic Acid/Methylfolate: Essential for preventing neural tube defects and supporting early cell division.
- Coenzyme Q10 (CoQ10): Helps support mitochondrial function in the egg, which is vital as we age.
- Vitamin D: Often called a pro-hormone, adequate levels are linked to better implantation rates.
3. Stress and Sleep
High levels of cortisol (the stress hormone) can inhibit the GnRH pulse generator in the brain, potentially delaying or stopping ovulation. Aim for 7–9 hours of quality sleep, as melatonin—the sleep hormone—is also a potent antioxidant that protects developing eggs.
Medical Interventions: When Science Lends a Hand
Sometimes, despite our best efforts, the biological machinery needs a tune-up. Modern medicine offers several pathways to boost fertility through targeted interventions.
Ovulation Induction
For women with irregular cycles or PCOS, medications like Letrozole or Clomiphene Citrate (Clomid) can be used. These oral medications gently nudge the ovaries to produce and release an egg, often under the supervision of an OB/GYN or endocrinologist.
Structural Corrections
In some cases, physical barriers prevent conception. Hysteroscopy or Laparoscopy can be used to remove uterine fibroids, polyps, or endometriosis lesions that might be interfering with implantation or blocking fallopian tubes.
Assisted Reproductive Technology (ART)
If more conservative measures don’t work, ART provides highly successful alternatives:
- IUI (Intrauterine Insemination): Concentrated sperm is placed directly into the uterus during ovulation.
- IVF (In Vitro Fertilisation): Eggs are retrieved, fertilised in a lab, and the resulting embryo is transferred back to the uterus.

When to See a Doctor: The Red Flags
Time is often a factor in reproductive health, and we want to ensure you aren’t waiting longer than necessary. The general rule is to seek help after one year of unprotected sex if you are under 35, or six months if you are 35 or older.
However, you should book an appointment immediately if you experience these “red flags”:
- Irregular or Absent Periods: This may indicate PCOS or premature ovarian insufficiency.
- Severe Pelvic Pain: Could be a sign of endometriosis or pelvic inflammatory disease.
- Two or More Miscarriages: Recurrent pregnancy loss requires a specialised workup.
- Known Male Factor Issues: If your partner has a history of testicular injury or surgery.
- History of STIs: Some infections can cause tubal scarring.
Frequently Asked Questions: Your Questions Answered
Does caffeine intake affect my fertility?
Moderate caffeine consumption (about 1 8-oz cup of coffee per day, or 200mg) does not appear to affect time to conceive significantly. However, high intake has been linked to a slightly increased risk of miscarriage, so it’s best to keep it in moderation.
Can lubricants prevent pregnancy?
Yes, many standard lubricants can act as a barrier or even be toxic to sperm. If you need lubrication, look for products labelled “sperm-friendly” or “fertility-friendly,” which are formulated to match the pH and consistency of fertile cervical mucus.
How much does age really matter for fertility?
While women are born with all the eggs they will ever have, and quality does decline over time (particularly after age 35), many women conceive healthy babies in their late 30s and early 40s. Age is just one piece of the puzzle; overall health and ovarian reserve are equally important.
Does the “legs up” trick after sex actually work?
There is no clinical evidence that lying with your legs in the air after intercourse increases the chances of pregnancy. Sperm are very fast swimmers and reach the cervix within seconds. However, if it makes you feel more relaxed, there is no harm in resting for a few minutes.
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding your specific health concerns or before starting any new supplement or treatment.