Hyperemesis Gravidarum vs Morning Sickness: Signs You Shouldn’t Ignore
Pregnancy nausea can be miserable, and for many of us, it can also be confusing. When does “normal” sickness become something more serious? If you’ve been searching for “hyperemesis gravidarum vs morning sickness, you’re likely trying to work out whether what you’re feeling is expected, or whether it needs medical help.
You are not overreacting for asking that question. We deserve clear answers, especially when we feel exhausted, worried, and unable to function. In this guide, we’ll walk through the difference between hyperemesis gravidarum vs morning sickness, why it happens, the signs to watch for, what can help, and when it’s time to call a doctor or midwife. Common pregnancy sickness is very common and usually settles by 20 weeks, but hyperemesis gravidarum is more severe, can cause dehydration and weight loss, and often needs medical treatment. (RCOG)
What is it?
“Morning sickness” is the everyday term for nausea and vomiting in pregnancy. Despite the name, it can happen at any time of day or night, not just in the morning. It usually starts early in pregnancy, often between weeks 4 and 7. (RCOG)
Earliest Signs of Pregnancy: What They Mean and When to Test
Morning sickness
Morning sickness usually means:
- nausea with or without vomiting
- reduced appetite
- symptoms that are unpleasant but still allow some food or fluids to stay down
- symptoms that often improve by around 16 to 20 weeks (MedlinePlus)
Hyperemesis gravidarum
Hyperemesis gravidarum, often shortened to HG, is the severe end of the spectrum. It means the nausea and vomiting are so intense that normal eating, drinking, and daily life become difficult. HG can lead to dehydration, weight loss, and electrolyte imbalance, and some women need outpatient rehydration or hospital care. It affects roughly 1 to 3 in 100 pregnancies. (nhs.uk)
In simple terms, the biggest difference in hyperemesis gravidarum vs morning sickness is not just feeling worse. It is whether your body is starting to struggle because you cannot keep enough fluid or nutrition down. (nhs.uk)
Why does it happen?
The exact cause is not fully understood, but pregnancy hormones appear to play a major role. Sources such as MedlinePlus link nausea and vomiting in pregnancy to rising hCG levels, while RCOG notes that some women may have stronger symptoms because of genetic differences and higher levels of the placental hormone GDF-15. (MedlinePlus)
You may be more likely to have worse symptoms if:
i: Higher-risk situations
- you’ve had HG or severe pregnancy sickness before
- you’re pregnant with twins or more
- there is a family history of HG,
- you are prone to motion sickness (nhs.uk)
None of this means you did anything wrong. This is not caused by weakness, stress, or “not coping well.” It is a real medical condition.
Folic Acid, Prenatal Vitamins, and What You Need Before Pregnancy
Evidence-Based Solutions
Medical interventions
Treatment depends on how severe the symptoms are and whether dehydration or weight loss has started.
i: For milder pregnancy sickness
- anti-sickness medicines prescribed in pregnancy can help
- doxylamine-pyridoxine is an established option; in the UK, Xonvea is the licensed formulation mentioned by RCOG
- other medicines used in pregnancy may include cyclizine, promethazine, prochlorperazine, metoclopramide, domperidone, or ondansetron, depending on the clinical picture and your doctor’s judgement (RCOG)
ii. For suspected hyperemesis gravidarum
You may need:
- assessment for dehydration and weight loss
- urine and blood tests
- intravenous fluids through a drip
- anti-sickness medicines by mouth, injection, or IV
- thiamine (vitamin B1), especially if vomiting is prolonged
- hospital admission if you cannot keep fluids or medicines down
- corticosteroids in more stubborn or severe cases after first-line treatment has not worked (RCOG)
This is one reason the hyperemesis gravidarum vs morning sickness question matters so much. HG is not something we should “push through” if we are becoming dehydrated or rapidly losing weight.
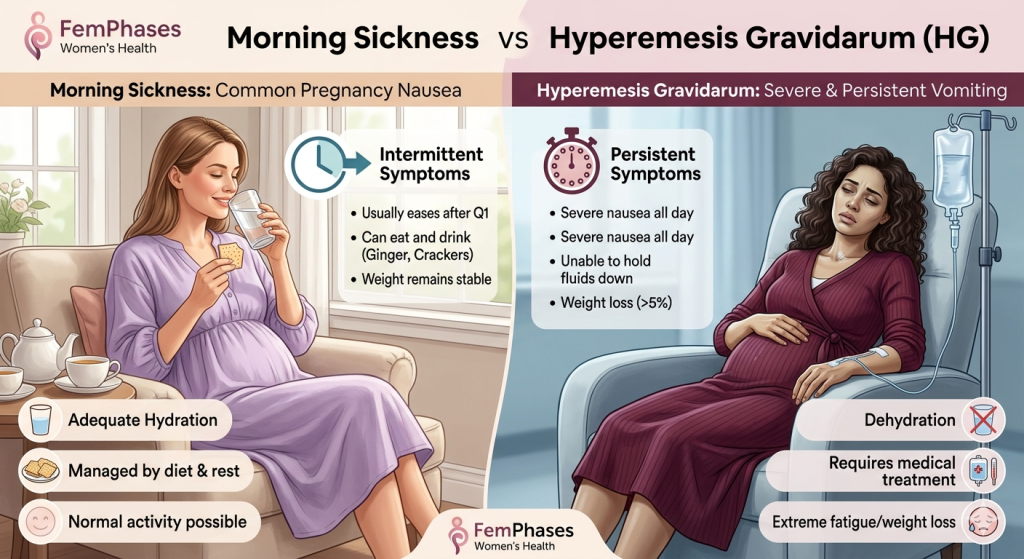
Signs or symptoms
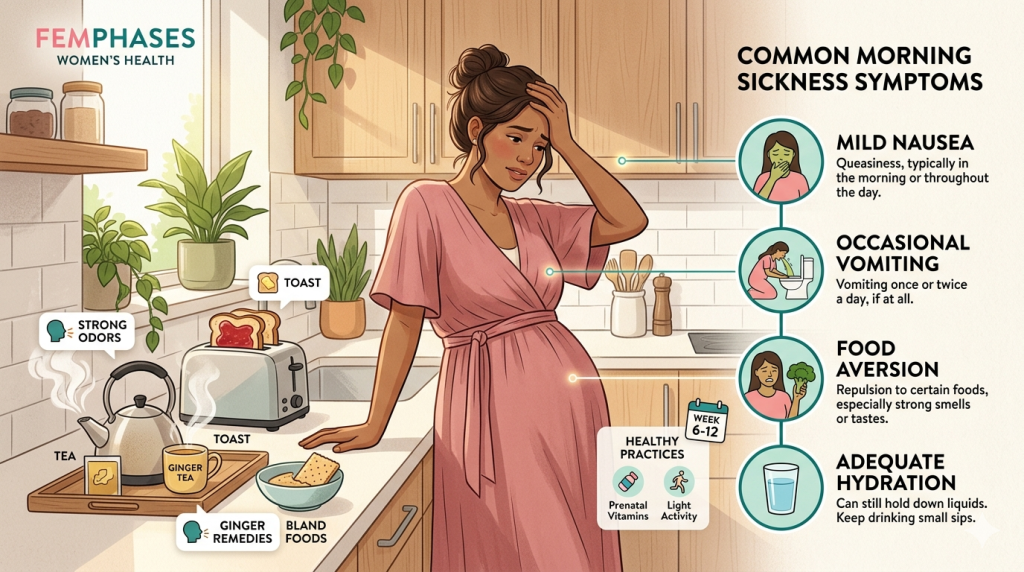
Morning sickness symptoms
- queasy feeling, often worse on waking, but possible any time
- occasional vomiting
- food aversions
- smell sensitivity
- still able to drink at least some fluids and eat small amounts (RCOG)
Hyperemesis gravidarum symptoms
- severe, persistent nausea
- frequent vomiting, sometimes many times a day
- inability to keep food or fluids down
- dark urine or peeing much less
- dizziness, weakness, or fainting
- weight loss
- feeling very dry, thirsty, or unwell
- symptoms continuing beyond the usual pattern, or becoming disabling (nhs.uk)
What is normal and when to pay attention
It is normal for pregnancy sickness to feel rough. It is not normal to be unable to function, unable to drink, or to feel as though your body is shutting down.
More likely to be “typical” morning sickness
- nausea without major dehydration
- vomiting, but still keeping some food and drinks down
- symptoms that are unpleasant but manageable at home
- gradual improvement by mid-pregnancy for many women (RCOG)
More concerning for HG or another medical issue
- not peeing much, or urine becoming very dark
- unable to keep food or fluids down for 24 hours
- rapid weight loss
- vomiting with dizziness or fainting
- vomiting blood
- abdominal pain, fever, or vomiting that starts after 16 weeks, because other causes may need to be ruled out (nhs.uk)
That is the heart of the difference between hyperemesis gravidarum and morning sickness: one is a common pregnancy sickness; the other is a more serious condition where your hydration, nutrition, and well-being may be at risk. (MedlinePlus)
Early Pregnancy Nutrition: What Matters in the First 12 Weeks
Holistic/Lifestyle Changes
These measures can help with milder symptoms and can still support recovery alongside medical care, but they are not a substitute for treatment if you are becoming dehydrated.
Nutrition and practical strategies
- eat small, frequent meals rather than large ones
- choose bland, lower-fat, carbohydrate-rich foods such as crackers, plain biscuits, rice, pasta, or potatoes
- avoid smells and foods that trigger nausea
- sip fluids little and often when you can tolerate them
- try eating and drinking during the times of day when nausea is less intense
- wear loose clothing if pressure on the stomach makes symptoms worse (RCOG)
Supportive reminders
- rest where possible
- pause iron tablets only if your clinician advises it, as iron can worsen sickness for some women
- seek emotional support if symptoms are affecting your mental health, because severe pregnancy sickness can be isolating and distressing (RCOG)
When to See a Doctor
Please seek medical advice promptly if:
- you cannot keep fluids down
- you have not peed in more than 8 hours, or your urine is very dark
- you feel faint, dizzy, weak, or confused
- you are losing weight
- you have severe vomiting
- you cannot keep your prescribed medication down
- you have abdominal pain, fever, or blood in your vomit
- your symptoms are affecting your ability to cope day to day (nhs.uk)
Get urgent help now
Seek urgent assessment the same day if you have signs of dehydration, fainting, blood in vomit, or you are unable to keep food or fluids down. (nhs.uk)

Key takeaway
If you are wondering about hyperemesis gravidarum vs morning sickness, the key question is this: Can you still drink, eat a little, and stay hydrated, or are you becoming depleted? Morning sickness is common and often manageable. Hyperemesis gravidarum is more severe, can cause dehydration and weight loss, and deserves medical care early. (RCOG)
Frequently Asked Questions
Q: Is hyperemesis gravidarum just very bad morning sickness?
A: Not exactly. HG is the severe form of pregnancy-related nausea and vomiting and can lead to dehydration, weight loss, and abnormal blood tests. (MedlinePlus)
Q: How do I know if I have hyperemesis gravidarum or normal morning sickness?
A: Think about hydration and function. If you are unable to keep fluids down, are losing weight, or feel dizzy and weak, it may be HG rather than typical morning sickness. (nhs.uk)
Q: Can hyperemesis gravidarum harm my baby?
A: Mild to moderate pregnancy sickness is not thought to harm the baby. Severe untreated HG can increase the risk of lower birthweight, which is why early treatment matters. (RCOG)
Q: When does morning sickness usually stop?
A: For many women, symptoms improve by 16 to 20 weeks, though some continue longer. HG may last beyond that and sometimes throughout pregnancy. (RCOG)
Q: What helps hyperemesis gravidarum?
A: Treatment may include anti-sickness medicines, IV fluids, thiamine, and sometimes hospital care or steroids if symptoms are severe. (RCOG)
Q: Should I go to hospital if I cannot stop vomiting in pregnancy?
A: Yes, especially if you cannot keep fluids down, are faint, or have signs of dehydration. (nhs.uk)
Medical disclaimer
This article is for general education and does not replace medical advice, diagnosis, or treatment. If you are pregnant and think you may have hyperemesis gravidarum, or you cannot keep fluids down, please get in touch with your doctor, midwife, maternity unit, or urgent care service promptly.








